Translate this page into:
Hospital-acquired acute kidney injury in medical, surgical, and intensive care unit: A comparative study
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Acute kidney injury (AKI) is a common complication in hospitalized patients. There are few comparative studies on hospital-acquired AKI (HAAKI) in medical, surgical, and ICU patients. This study was conducted to compare the epidemiological characteristics, clinical profiles, and outcomes of HAAKI among these three units. All adult patients (>18 years) of either gender who developed AKI based on RIFLE criteria (using serum creatinine), 48 h after hospitalization were included in the study. Patients of acute on chronic renal failure and AKI in pregnancy were excluded. Incidence of HAAKI in medical, surgical, and ICU wards were 0.54%, 0.72%, and 2.2% respectively (P < 0.0001). There was no difference in age distribution among the groups, but onset of HAAKI was earliest in the medical ward (P = 0.001). RIFLE-R was the most common AKI in medical (39.2%) and ICU (50%) wards but in the surgical ward, it was RIFLE-F that was most common (52.6%). Acute tubular necrosis was more common in ICU (P = 0.043). Most common etiology of HAAKI in medical unit was drug induced (39.2%), whereas in surgical and ICU, it was sepsis (34% and 35.2% respectively). Mortality in ICU, surgical and medical units were 73.5%, 43.42%, and 37.2%, respectively (P = 0.003). Length of hospital stay in surgical, ICU and medical units were different (P = 0.007). This study highlights that the characters of HAAKI are different in some aspects among different hospital settings.
Keywords
Epidemiology
hospital acquired acute kidney injury
mortality
RIFLE criteria
Introduction
Acute kidney injury (AKI), previously termed “acute renal failure” (ARF), is a common and serious disease. There has been a frequent change in definition of the KI.[1] Acute Dialysis Quality Initiative (ADQI), proposed consensus definition and stage of ARF known as RIFLE criteria (Risk, Injury, Failure, Loss, and End-stage kidney disease) in 2002.[2] Subsequently, the Acute Kidney Injury Network (AKIN) proposed the term ‘Acute Kidney Injury’(AKI) to reflect the entire spectrum of ARF.[3]
With the changing definition, the epidemiology of AKI has changed. AKI, particularly in hospitalized patients, is associated with significant morbidity and mortality.[4–6] However, most epidemiologic studies on AKI were compartmentalized into 2 entities: (i) hospital-acquired AKI (HAAKI) and (ii) community-acquired AKI (CAAKI).[67] Studies on HAAKI were mostly centered around the critically ill ICU patients or only on some specific sub-groups of medical and surgical patients.[89] There are few comparative studies of HAAKI in medical, surgical, and ICU patients.[1011] HAAKI is quite common in this part of the country.[1213] Therefore, this comparative study was conducted to know the epidemiological and clinical profiles of AKI in surgical, medical, and ICU units at our centre.
Materials and Methods
This study was carried out during the period from December 2009 to April 2011. Institute's ethical committee approval was obtained prior to the study and an informed consent was taken from all patients. It was presumed that the patient had normal renal function if the serum creatinine at admission was <1.5 mg/dl or urine output was >0.5 ml/kg/h. AKI was defined using the RIFLE criteria based on serum creatinine.[2] HAAKI was defined as the development of AKI any time after 48 h of hospitalization, on a patient who was admitted with normal renal function. This arbitrary time of 48 h was used to allow subclinical CAAKI to manifest. To classify patients into one of the RIFLE criteria, peak and baseline (at the time of admission) creatinine values were collected from the patient case sheet. The peak creatinine was defined as the highest serum creatinine level during hospital admission. Adult patients, ≥18 years of age, regardless of gender, who fulfilled the criteria of HAAKI were included. Patients of acute on chronic renal failure, CAAKI, and pregnant women developing AKI were excluded clinical and laboratory data was collected for all patients. All relevant data of the patients like the primary disease for which the patient was admitted, medication, operative or invasive procedure, complications during the course of hospital stay, and co-morbidities were noted.
The most probable causes of HAAKI were assigned as given below:
-
Nephrotoxic drugs: If a patient had received a drug with known nephrotoxic potential for a minimum period of two days prior to the defined increase in serum creatinine concentration.[12]
-
Sepsis: When two or more of the following were present as a result of systemic infection; (1) temperature >38.0 or <36.0°C; (2) heart rate >90/min; (3) respiratory rate >20/min or pco2 < 32 mm, and (4) white blood cell count >12,000/mm3 or <4000 mm3, or >10% band form.[14]
-
Hypotension: If there was overt/orthostatic hypotension (BP <80 mm hg), because of purely cardiovascular cause.[15]
-
Volume loss: If there was obvious cause of volume depletion along with loss of skin turgor with decrease of more than 5% of body weight.[15]
-
Sepsis and drugs: If there were sepsis as well as use of drugs which are potentially nephrotoxic.[16]
-
Volume loss and sepsis: When there was volume loss as well as septicemia.[16]
-
Sepsis-drugs – hypotension: If there was septicemia, use of drugs which are potentially nephrotoxic as well as hypotension, because of cardiovascular cause.[16]
HAAKI was also divided into three anatomical groups: (a) Pre-renal, (b) Renal: Acute tubular necrosis (ATN), and acute interstitial nephritis (AIN) etc., and (c) Post-renal.[17] ATN was diagnosed based on clinical background with support from laboratory evidences and pattern of recovery of renal function with treatment.
Patients were followed-up daily until the last day of hospital stay but follow-up after the discharge was not included in the study. Serial records of urine output and serum creatinine were maintained. Renal replacement therapy was instituted according to standard clinical indications. Outcomes of HAAKI in this study were measured in terms of: (1) length of hospital stays (LOS) – defined as the number of days from admission to discharge, death, or left against medical advice from hospital, and (2) treatment outcome: dies or discharged with improved renal function. Complete recovery was defined as coming down of the serum creatinine to <1.5 mg/dl along with improvement in urine output during the hospital stay. On the other hand, partial recovery of renal function was defined as the improvement in renal function (as determined by an increase in urine output and a decrease in serum creatinine) but serum creatinine levels still >1.5mg/dl at the time of discharge from the hospital.
Variables were reported as mean ± SD. Statistical calculation was done using Analysis of Variance (ANOVA) and Chi-square test. P < 0.05 was considered significant. All the calculations were carried out with the help of software SPSS16 version.
Results
There were 9413, 10532, and 1504 admissions in medical ward, surgical ward, and ICU unit respectively. The incidence of HAAKI in medical, surgical, and ICU unit were 0.54% (n = 51), 0.72% (n = 76) and 2.2% (n = 34), respectively (P = 0.005). The most common age-group of HAAKI in all the three units was 50-65 years. The age in the medical, ICU, and surgical wards were 50.13 ± 15.4, 50.7 ± 18.42, and 54.2 ± 18.0 years respectively. However, there was no significant difference in the age of the patients among the three units (P = 0.37).
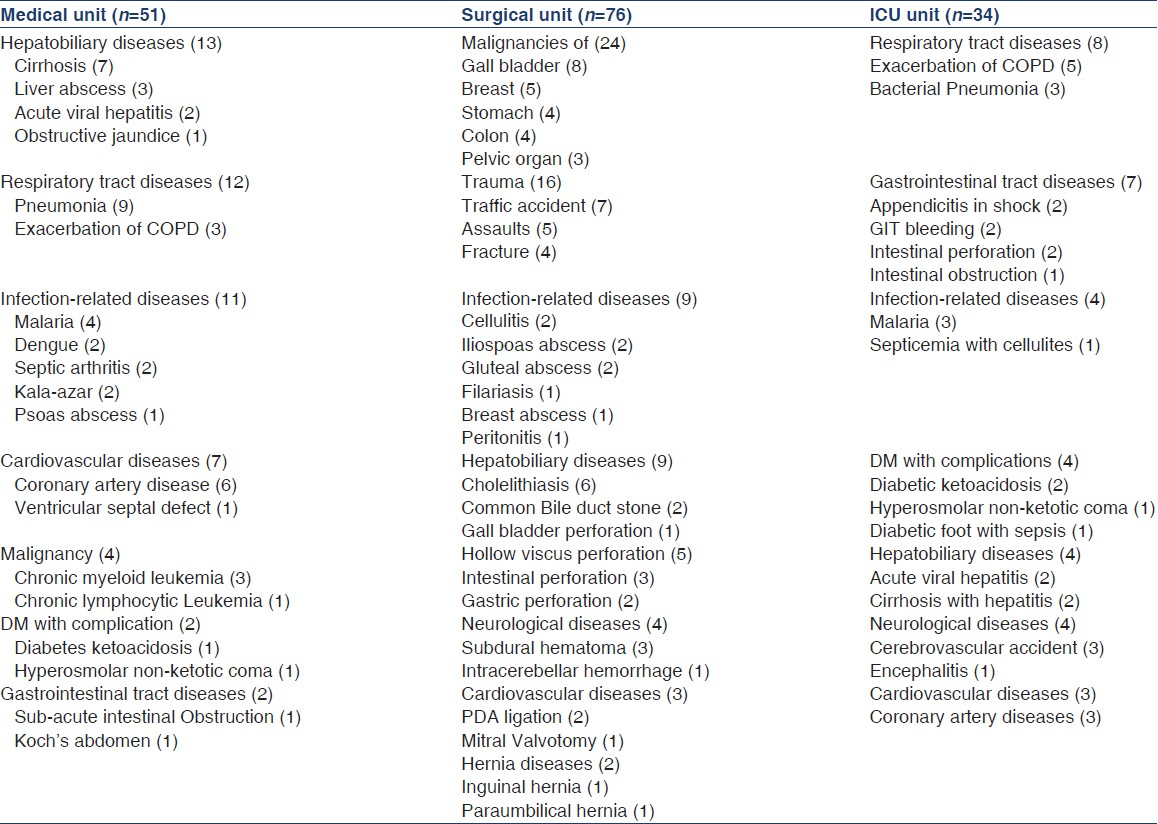
Two most frequent primary diseases at the time of admission into the medical ward were hepatobiliary diseases (n = 13, 25.49%) and respiratory tract diseases (n = 12, 23.52%). This was closely followed by infection-related diseases (21.56% n = 11). The most common primary disease at admission into surgical unit was malignancies, comprising 31.57% (n = 24). Respiratory tract diseases was the commonest reason for admission into ICU (n = 8, 23.5%). Table 1 shows the primary diseases of admission into the different units of the hospital.
Onset of HAAKI was earliest in medical unit (6.04 ± 2.55 days). In ICU patients, HAAKI developed over 8.44 ± 6.53 days whereas in surgical wards that was 12.09 ± 9.60 days. On statistical analysis, there was a significant difference in the onset of HAAKI among the three units (P < 0.001). Oliguria was noted in 47%, 57.89%, and 61% of the patients at the time of diagnosis of AKI in medical, surgical, and ICU unit patients respectively. The most common cause of HAAKI was sepsis in surgical (n = 26, 34%) and ICU ( n = 12, 35.2%) unit whereas drugs were the culprit in medical unit (n = 20, 39.2%). Among the drugs, the most common was amino-glycoside (9/20). Volume depletion contributed to AKI in 17.8% and 14.7% of cases in the medical and ICU units respectively. Thus, sepsis, volume loss, and drugs were the main cause of HAAKI in all the units, either alone, or in combination [Table 2].

RIFLE-R was the most common category of HAAKI in both the medical and ICU unit (n = 20, 39.2% and n = 17, 50% respectively), whereas RIFLE-F was the most common category in the surgical unit (n = 40, 52.6%) [Table 3]. One case of RIFLE-L was seen in the surgical unit. Statistical analysis showed significant difference among the different categories of RIFLE in three units (P = 0.043). Pre-renal was the most common form of HAAKI in both the medical and surgical units (n = 24, 47.05% and n = 39, 51.31%, respectively) whereas ATN and pre-renal were shared equally (50% each) in ICU. Acute interstitial nephritis as a cause of HAAKI was seen in 13.7% of the cases in the medical unit. Dialysis support was needed in 35.52%, 25.49% and 20.58% of cases in surgical, medical and ICU units respectively.

Mortality of HAAKI patients was highest in ICU (n = 25, 73.5%) followed by surgical (n = 33, 43.4%) and medical (n = 19, 37.2%) ward respectively. On statistical comparison, mortality rate was significantly different among the three units (P = 0.003). In the medical unit, mortality was highest in RIFLE-I (36.84%, n = 7) followed by RIFLE-R and RIFLE-F category equally (31.57% each). In the surgical unit, most of the deaths occurred in the F category (66.6%, n = 22), whereas in the ICU, maximum number of deaths observed was in RIFLE-R (52%, n = 13). Categories-wise mortality and renal function recovery in the three units are shown in Table 3. LOS was longest in the surgical ward (19 ± 9.79 days) in comparison to that of medical (14.29 ± 5.1 days) and ICU (17.4 ± 8.96 days) units. LOS was significantly different in patients with HAAKI among the three units of hospital (F = 5.186, P = 0.007). Table 4 summaries the differences of main parameters among the three units.

Discussion
HAAKI is a common and serious complication in hospitalized patient and can affect any section of age, gender, geographic region, or religion.[45] In our study, we observed an incidence of 0.54%, 0.72%, and 2.2% of HAAKI in medical, surgical, and ICU units respectively. Higher incidence of AKI in ICU patients may be due to a more severe nature of the primary illness. Similar incidences of HAAKI were reported from other Indian studies.[1213] However, a slightly higher incidence of AKI in hospitalized patients was observed from other centers (between 1% and 4.9%).[71819] The lower incidence of HAAKI in our patients may be due to the improvement in the health-care system and effective treatment modalities in comparison to earlier decades. In this study, it was found that there was no significant difference (P = 0.37) in the age distribution of the patients among the three units, indicating that no age is immune to HAAKI with respect to place of admission.
The primary disease on which the patients developed HAAKI in different units was heterogeneous as per the hospital admission protocol, disease prevalence in community, as well as susceptibility to HAAKI. In medical units, hepatobiliary diseases were the most common primary disease at admission (25.49%) among the HAAKI patients followed by respiratory tract diseases (23.5%). De Mendonca et al., also observed a similar pattern of underlying primary disease.[20] In the present study, malignancies (31.57%) accounted for the most common primary disease in the surgical unit. This is in contrast to other studies, where HAAKI were more common in surgery of non-malignant conditions like surgery of abdominal organ, cardiac, or vascular system.[2122] Our hospital is a tertiary care hospital and we get complicated cases referred by the peripheral physician for management. This might be the reason for a high incidence of malignancy in the surgical unit. In ICU patients, respiratory tract disease (23.52%) was the most primary disease at admission that developed HAAKI. This finding is similar with that of de Mendonca et al., who found various medical and surgical patients in ICU admission.[21]
The time of onset of HAAKI was earliest in the medical unit in comparison to other units (P < 001). Combination of volume loss, hypotension, ‘volume loss-sepsis’, and ‘sepsis-drug-hypotension’ constitutes 37.5% of HAAKI patients in medical but it was only 18.3% in surgical and 33% in ICU unit. The early onset of AKI in medical set-up may be due to more meticulous physical examination including urine output and regular early laboratory investigation (serum creatinine).
Higher incidence of oliguria in ICU (61%) in comparison to surgical (57.89%) and medical unit (47.05%) may be due to a higher incidence of ATN (50%) and multi-organ failure in this unit in comparison to that of others.
The most common cause of a HAAKI in the medical unit was drug toxicity (39.2%), whereas sepsis was the commonest cause in surgical and ICU. This difference may be due to fact that surgical and ICU patients are usually more prone to infection because of frequent use of more invasive procedures like ventilator supports, instrumentation, central line insertion, exposed wounds, and surgical wounds infection. This finding was in accordance with other studies where drugs contributed to 29-47.7% of HAAKI.[121823] Our finding of higher incidence of sepsis as causes of HAAKI in surgical and ICU unit (34% and 35.2% respectively) was similar to that of Uchino et al.[4] and Prakash et al.[24]
In our study, volume depletion was accountable for 17.8%, 14.7%, and 9.2% causes of HAAKI in medical, ICU, and surgical units respectively. This difference may be due to the fact that patients admitted into the medical and ICU wards are usually sicker and often had a decreased level of consciousness, leading to decreased oral intake than that of surgical ward where 50% of the admissions were elective in nature with proper patient selection. Hypotension was the fourth leading cause of HAAKI in the medical and ICU patients (7.8% and 11.7% respectively), whereas it accounted for AKI in 2.6% of the surgical patients. It may be a reflection of the general patterns of patient's admission, whereas the patients with cardiovascular diseases are usually admitted either into the medical or in ICU units whereas in the surgery units, most of admissions are elective in nature.
The need for dialysis was more in surgical patients in comparison to that of ICU and medical units. This may be a reflection of the higher incidence of RIFLE-F categories of patients in surgical unit than in the other units. We noted that 25.49%, 35.1%, and 20.58% of HAAKI patients required dialysis in medical, surgical, and ICU units respectively. Other previous studies found dialysis requirement in 7.7-19% of HAAKI,[71622] and this lower incidence may be due to difference in the criteria for initiation of dialysis and heterogeneity of patients population.
Mortality was the highest in ICU (73.5%) which was statistically significant in comparison to that of the other two units (P = 0.003). This higher incidence may be partly due to the high percent of multiple organ involvement in the ICU patients. In general, indication for ICU admission itself also is an indicator of the severity of primary illness which directly influences the mortality rate. The overall mortality in three units was 51.3%, which was quite similar (51%) to that of Biradar et al.[23] Similar to our finding, the reported rate of mortality of HAAKI ranges from 25% to 70%.[6715] Mortality in ICU in this study was in accordance with earlier studies where that ranges from 60.3 to 76.2%.[42425] The mortality in the medical unit (37%) was higher in contrast to other studies (14-24.8%).[20222326] However, Chamberlain et al., also reported a 59% mortality rate.[27] These differences may be due to variation in the primary disease, socio-economical status, and state of health-care of the population. As our hospital is a tertiary center, we admit only the more sick patients who may contribute to a higher death rate. Mortality of HAAKI patients in surgical unit was 43.4%. Nash et al., observed a mortality of 37.5% in HAAKI patients in postoperative cases.[26] This may be due to the difference in the set of study population.
Among the various RIFLE categories, mortality of HAAKI was different in the three units (medical, surgical, and ICU) of the hospital. In ICU, maximum deaths were in RIFLE-R (52%) and it could be explained by the fact that not only severity of renal failure, but primary disease is also a strong determinant of the disease outcome. In surgical units, mortality was highest in RIFLE-F (66.6%) which can be explained on the basis of severity of AKI, whereas in the medical unit that was in RIFLE-I (36.84%). To best of our knowledge, there have not been any major studies using RIFLE criteria for comparing the mortality among the hospital- acquired AKI cases of medical, surgical, and ICU set-ups simultaneously. Statistically significant difference in LOS among the three units with the longest in surgical unit observed in this study may be due to variation in the distribution of cases in different RIFLE categories. In surgical units, most patients were in RIFLE-F, thus explaining the longer stay in hospital (P = 0.007). Mean length of hospital stay of total HAAKI patients in our study was 17.27 days which was consistent with that of other studies.[2327]
Conclusion
The clinical and epidemiological characters of HAAKI in medical, surgical, and ICU are different from each other in certain aspects. This is mainly contributory to the unit-specific factors and disease characters of the underlying primary disease. HAAKI develops earlier in medicine when compared to other units. At the time of diagnosis of HAAKI, oliguria was more common in ICU patients. ATN and pre-renal was equally responsible for the development of HAAKI in ICU. However, pre-renal was the most common form of HAAKI in both the medical and surgical units. Among the RIFLE categories, RIFLE-R was the more common category of HAAKI in both the medical and ICU units, whereas RIFLE-F was the most common category in surgical unit. Mortality was the highest in ICU followed by surgical and medical units respectively. Medical unit patients recovered early from the illness and were more tolerant to HAAKI.
Source of Support: Nil
Conflict of Interest: None declared.
References
- Developing a consensus classification system for acute renal failure. Curr Opin Crit Care. 2002;8:509-14.
- [Google Scholar]
- Acute renal failure-definition, outcome measures, animal models, fluid therapy and information technology needs: The Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care. 2004;8:R204-12. [Last accessed 2011 Oct 23]
- [Google Scholar]
- Acute Kidney Injury Network: Report of an initiative to improve outcomes in acute kidney injury. 2007. Crit Care. 11:R31. Available from: http://ccforum.com/content/11/2/R31
- [Google Scholar]
- Acute renal failure in critically ill patients: A multinational, multicenter study. JAMA. 2005;294:813-8.
- [Google Scholar]
- Epidemiology and outcomes of acute renal failure in hospitalized patients: A national survey. Clin J Am Soc Nephrol. 2006;1:43-51.
- [Google Scholar]
- Acute renal failure in intensive care units–causes, outcome, and prognostic factors of hospital mortality; a prospective, multicenter study. French Study Group on Acute Renal Failure. Crit Care Med. 1996;24:192-8.
- [Google Scholar]
- Hospital-acquired renal insufficiency: A prospective study. Am J Med. 1983;74:243-8.
- [Google Scholar]
- Acute kidney injury in the intensive care unit: An update and primer for the intensivist. Crit Care Med. 2010;38:261-75.
- [Google Scholar]
- North East Italian Prospective Hospital Renal Outcome Survey on Acute Kidney Injury (NEiPHROS-AKI): Targeting the problem with the RIFLE Criteria. Clin J Am Soc Nephrol. 2007;2:418-25.
- [Google Scholar]
- The spectrum of acute renal failure in the intensive care unit compared with that seen in other settings. The Madrid Acute Renal Failure Study Group. Kidney Int Suppl. 1998;66:S16-24.
- [Google Scholar]
- Acute renal failure in medical and surgical intensive care units: A one year prospective study. Ren Fail. 2003;25:105-13.
- [Google Scholar]
- Spectrum of hospital-acquired acute renal failure in the developing countries: Chandigarh study. Q J Med. 1992;83:497-505.
- [Google Scholar]
- Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest. 1992;101:1644-55.
- [Google Scholar]
- Risk factors and outcome of hospital-acquired acute renal failure. Clinical epidemiologic study. Am J Med. 1987;83:65-71.
- [Google Scholar]
- Treatment related acute renal failure in elderly: A hospital based prospective study. Nephrol Dial Transplant. 2000;15:212-7.
- [Google Scholar]
- Acute renal failure in the hospital: Diagnosis and management. Hosp Physician. 2006;3:51-8.
- [Google Scholar]
- Cause and prognosis of acute renal failure in Kuwait: A 2-year prospective study. J Trop Med Hyg. 1989;92:325-9.
- [Google Scholar]
- Acute renal failure in the ICU: Risk factors and outcome evaluated by the SOFA score. Intensive Care Med. 2000;26:915-21.
- [Google Scholar]
- Etiology, incidence, and prognosis of renal failure following cardiac operations. Results of a prospective analysis of 500 consecutive patients. J Thorac Cardiovasc Surg. 1976;71:323-33.
- [Google Scholar]
- Clinical spectrum of hospital acquired renal failure: A study from tertiary care hospital. Indian J Nephrol. 2004;14:93-6.
- [Google Scholar]
- Acute renal failure in the intensive care unit. J Assoc Physicians India. 2006;54:784-8.
- [Google Scholar]
- Spectrum of acute renal failure and factors predicting its outcome in an intensive care unit in India. Ren Fail. 2006;28:119-24.
- [Google Scholar]







