Translate this page into:
Maternal, fetal and renal outcomes of pregnancy-associated acute kidney injury requiring dialysis
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Pregnancy-associated acute kidney injury (PAKI) is encountered frequently in developing countries. We evaluated the maternal, fetal and renal outcomes in women with PAKI who needed at least one session of dialysis. Of the total of 98 cases (mean age 28.85 ± 5.13 years; mean parity 2.65 ± 1.28) of PAKI, the most common cause of PAKI was postabortal sepsis. Eighteen patients died; those with oligoanuria, sepsis and central nervous system (CNS) involvement were at greater risk of mortality. The relative risk (RR) of neonatal mortality was lower after with full-term delivery (RR: 0.17, 95% confidence interval (CI): 0.03-0.96, P = 0.02) compared to preterm delivery. Of the 80 surviving patients, 60 (75%) patients achieved complete recovery of renal function at the end of 3 months; and of the remaining 14 had presumed (n = 4) or, biopsy-proven (n = 10) acute patchy cortical necrosis. The RR of non-recovery of renal function was high (RR: 24.7, 95% CI: 3.4- 179.5) in patients who did not recover at 6 weeks. Of the 14 patients with cortical necrosis, 3 (21.42%) became independent of dialysis at 6 months. PAKI patients should be watched for dialysis independency for 6 months.
Keywords
Acute cortical necrosis
acute kidney injury
dialysis
outcomes
pregnancy
Introduction
Pregnancy-associated acute kidney injury (PAKI) is associated with increased maternal morbidity and mortality. The maternal mortality associated with PAKI has been reported from 9% to 55%.[12] The incidence of PAKI has decreased in developed countries over the last 60 years from 1 in 3000 in the mid-20th century to 1 in 20,000.[3] However, PAKI still comprises 25% of referrals to dialysis center in developing countries.[4] The incidence ranges from 4.3% to 14.5% in India.[56] Septic abortion as a cause of PAKI decreased from 33.3% in 1980-1985 to 6.3% in 1989-1997; however, it still remains the most common cause of PAKI in developing countries.[1] Worldwide, one of the major causes of sepsis leading to PAKI is illegal abortion. At least 5% of women undergoing illegal abortions become gravely ill.[7] Puerperal sepsis and postpartum hemorrhage are the leading causes of acute tubular necrosis (ATN) in the postpartum period.[8] Renal cortical necrosis, a rare and irreversible cause of AKI, accounts for about 2% of all cases of AKI; and 50-70% of these cases are associated with complications of pregnancy.[9]
A transient decline in glomerular filtration rate with pregnancy-associated complications is not uncommon. It occurs once in 8000 deliveries while PAKI requiring dialysis occurs in approximately 1 in 20,000 pregnancies.[10] Recent studies have shown that patients in the risk and injury groups on RIFLE criteria of AKI had good outcome as compared to the failure group.[1112] We undertook this study to analyze the etiologies, risk factors and outcomes of PAKI patients requiring dialysis.
Materials and Methods
This was a retrospective study. Data of all the cases of AKI referred to our nephrology department between January 1, 2006 and December 31, 2011 were screened. Patients were defined for AKI as per RIFLE criteria.[12] The inclusion criteria was AKI with requirement of at least one session of dialysis in otherwise healthy female following pregnancy, abortion, delivery of fetus, and related to its complication directly but not from any other cause. Pregnancy in renal transplant recipients, patients with previous history of renal diseases, diabetes mellitus or hypertension prior to pregnancy, and those with small or unequal kidneys on ultrasound or any evidences of chronic kidney diseases were excluded from the study. The demographic profile and clinical characteristics of the patients in terms of age, parity, educational status, family income, access to antenatal care, duration of gestation, type and place of delivery, fetal outcome, duration of symptoms prior to admission, urine output, hematological and biochemical profiles, renal replacement therapy, duration of hospitalization, report of kidney biopsy if done, recovery of renal function and patients survival were recorded. Kidney biopsy was done if patients did not show any signs of recovery of renal function after 4 weeks of AKI.
Sepsis was defined as per the criteria of systemic inflammatory response syndrome laid down by American College of Chest Physicians.[13] CNS involvement was considered if the patients had altered sensorium and/or had seizure at time of presentation. Hepatic dysfunction was considered if the patients had increased alanine transaminase and serum bilirubin. The outcome of pregnancy was noted in terms of abortion, preterm alive or dead fetus, full-term alive or, dead fetus. Preterm delivery was defined by delivery before the 37 completed weeks of pregnancy. The renal recovery was analyzed in terms of achievement of normal renal function at the time of discharge, dialysis dependent and independent state of the patients. The study was approved by the ethics committee of the institute.
Statistical analysis
All data are presented as mean ± standard deviation. Proportions were compared using the Chi-square test or Fischer exact test. Student's t-test was used to compare the means between the two groups. The relative risk (RR) of mortality with 95% confidence interval with different organ involvement was analyzed. The RR of mortality was calculated comparing the patients with the involvement of the particular organ versus patients without involvement of that organ in the patients. P < 0.05 was considered significant. Data were analyzed using SPSS 15.0, Chicago, USA.
Results
Demographic profiles and clinical characteristics
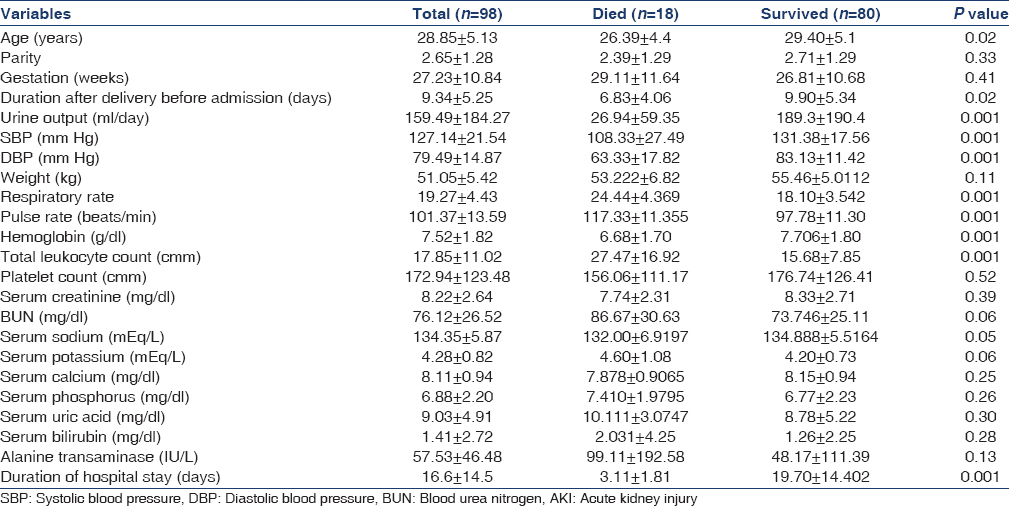
Of the total 2890 cases of AKI during the study period, 98 (3.39%) had PAKI and received at least one session of dialysis. The demographic, clinical and biochemical characteristics at presentation are shown in Table 1. The mean age was 28 ± 5 years. A total of 29 (29.6%) were <25 years of age; 53 (54.08%) were between 25 and 35 years old, and 16 (16.32%) were >35 years. Twenty (20.4%) patients were primigravida and 78 (79.60%) multigravida. The mean parity was 2.65 ± 1.28, and mean duration of gestation was 27.23 ± 10.84 weeks. Fifteen patients (15.3%) developed PAKI in first trimester of pregnancy, 28 (28.57%) in second trimester and 55 (56.12%) in third trimester of pregnancy. Sixty-three PAKI cases had antenatal care with local obstetrician and 35 did not have any antenatal check-up.
Etiologies and clinical manifestations of pregnancy-associated acute kidney injury
The etiologies of PAKI are shown in Table 2. The most common cause was sepsis. Twenty-five (25.51%) developed sepsis after abortion by local village practitioners or traditional birth attendants, 7 (7.14%) after medical termination of pregnancy (MTP) at primary health centers, and 23 (23.46%) had puerperal sepsis. Twenty-three (23.46%) developed PAKI following upon antepartum and postpartum hemorrhage, 14 (14.28%) after pre-eclampsia/eclampsia, 4 (4.08%) after hemolysis, elevated liver enzymes and low platelet (HELLP) syndrome, and 2 (2.02%) had postpartum hemolytic uremic syndrome.

Of all the cases of PAKI, 44 (44.90%) presented within 1 week, 30 (30.61%) presented between 1 and 2 weeks and 24 (24.49%) presented ≥2 week after abortion/delivery. Thirty-four (34.7%) of them had lower segment cesarean section and 64 had vaginal delivery. Eighteen (18.37%) patients had retained product of conception at presentation, which needed surgical removal. Seven (7.14%) presented with shock, 54 (55.10%) had high-grade fever, 8 (8.20%) had seizure, 51 (52.04%) had severe anemia with hemoglobin level <6 g/dl requiring immediate blood transfusion, 14 (14.29%) had clinical jaundice and 23 (23.47%) had transaminitis.
Maternal and fetal outcomes
Of the 98 patients with PAKI, 18 (18.36%) patients died. The cause of death was sepsis in 13 patients (10 with disseminated intravascular coagulation and multiorgan failure, and three with refractory septic shock), myocarditis and refractory cardiac arrhythmia in two, HELLP syndrome, cerebrovascular accident, and sudden death in one each. The RR of mortality with other organ dysfunction is shown in Table 3. Patients with oligoanuria, sepsis and CNS involvement were at greater risk of death. The RR of mortality was not increased in patients with hepatic dysfunction and thrombocytopenia. The patients who received single session of dialysis were at greater risk of mortality than those who received multiple session of dialysis. Of all the 98 patients with PAKI, 46 (46.94%) had either medical or illegal abortion, 9 (9.18%) had preterm delivery and 43 (43.8%) had full-term delivery. Of the nine neonates with preterm delivery, only 5 (55.56%) survived. Of the 43 neonates after full-term delivery, 36 (83.7%) survived. The RR of neonatal mortality with full-term delivery was lower (RR: 0.17, 95% confidence interval (CI): 0.03-0.96, P = 0.02) than that after preterm delivery.

Renal outcomes
Of all the patients, 24 (24.49%) had required one session of dialysis while 74 (75.51%) required multiple (6 ± 5, range 1-30) sessions of dialysis. Kidney biopsy was performed in 16 patients: 8 patients had patchy cortical necrosis, 2 had patchy cortical necrosis with thrombotic microangiopathy and 6 had ATN.
Eighty (81.63%) patients were available for renal outcome analysis: 60 (75%) became dialysis independent, and 20 (25%) remained dialysis-dependent at 6 weeks (P = 0.001).
Of these, 10 had biopsy proven acute patchy cortical necrosis; 4 patients had presumed acute cortical necrosis; and the remaining 6 patients had biopsy proven severe ATN who recovered their renal function completely (serum creatinine <1.4 mg/dl). At the end of 6 months follow-up, of the 10 patients with biopsy proven acute patchy cortical necrosis, 2 became dialysis-free with serum creatinine of more than 3 mg/dl and 8 remain dialysis-dependent; and of the 4 patients with presumed acute cortical necrosis, only 1 became dialysis-free with serum creatinine more than 3 mg/dl. Overall, 3 out of 14 (21.42%) became dialysis-free and 11 (78.58%) remained dialysis-dependent at 6 months (P = 0.02). Both of the patients with patchy cortical necrosis and thrombotic microangiopathy remained dialysis-dependent despite being treated with plasmapheresis. The risk ratio of non-recovery of renal function was higher (RR: 24.7, (95% CI: 3.4-179.5) in patients who did not recover at 6 weeks.
Discussion
In this study, we observed that 18.36% PAKI patients requiring dialysis died. Those who died were younger, had lower systolic and diastolic blood pressures, greater pulse rates and respiratory rates at admission. The number of dialysis and duration of hospital stay was significantly less in patients who died as compared to those who survived. The reason was the late referral of these patients in critically sick condition with multiorgan dysfunction. Like in non-PAKI patients,[14] the RR of mortality was significantly greater in patients with sepsis, CNS involvement and oliguria at presentation. Hepatic dysfunction and thrombocytopenia was not associated with increased risk of mortality in our study while these factors have been associated with maternal mortality in another study.[15]
With increasing availability of medical services, better antenatal and postnatal care and provisions for MTP, the incidence of PAKI is decreasing in India [Table 4].[5681516] The incidence of PAKI decreased from 38.62% in 1987 to 9% in 2008[513] and 3.39% in present study, which included only PAKI patients requiring dialysis. However, the rate of PAKI in India is still very high compared to that of the developed countries (1-2.8%).[171819] Stratta et al. quoted that the incidence of obstetrical AKI decreased from 43% (1956-1967) to 0.5% with respect to total AKI cases (1988-1994) and no case of maternal death or irreversible renal damage was observed in the last 7 years.[20] Pre-eclampsia, eclampsia, HELLP and hemolytic uremic syndrome remain the leading causes of PAKI in developed countries and the decline in PAKI is mainly because of significant decrease in abortion and infection-related complications.[192021] A study from Casablanca reported that pre-eclampsia and eclampsia accounts for 74.5% cases, sepsis in 11% and hemorrhages for 7.2% PAKI cases.[19] Contrary to the developed countries, postabortal sepsis remains the most common cause of PAKI in India and accounts for about a quarter of all cases in our study. The varying incidence as low as 9.76% to as high as 59.7% of postabortal sepsis causing PAKI has been reported in literature from India.[612] In terms of association of PAKI with duration of pregnancy, previous study published in 1976 showed that majority of PAKI (59.7%) occurs in early pregnancy,[21] while the present study and another recent study from India showed greater incidence of PAKI in late pregnancy.[15] This appears to be due to the legalization of abortion, which allows safe and early MTP in India.

The high maternal mortality in India is still a great social, economical and medical concern. The maternal mortality of 18.36% in our study is similar to other studies reported from India ranging from 18% to 24%.[615] A study from a developed country reported maternal mortality of 9.1% in case of PAKI, which is almost half of that reported from India. The greater mortality in many developing countries, including India, compared to developed countries is mainly because of greater sepsis-related death.[22232425] The fetal death of only 5.5% has been reported in case of PAKI in a study from a developed country. After excluding cases of abortions a fetal mortality of 26.19% was observed in our study, similar to that reported in pregnant women admitted in ICU with renal failure.[22] The high fetal mortality may be because of poor antenatal care and high rate of illegal abortion in our study. This reflects poorly on socioeconomic condition, ignorance and lack of medical facilities in this part of the world.
The other important observation in our study was that the recovery of renal function was poor in patients who remain dialysis-dependent at 6 weeks of PAKI. The late recovery of renal function and dialysis independency at 6 months follow-up in patients who were dialysis-dependent at 3 months suggest that these patients should be watched for up to 6 months for recovery of some degree of renal function. The percentage of patients who did not recover their renal function in our study was either similar or relatively better than that reported from other part of countries.[151617] Similar to our study, Goplani et al. showed that of the 81.42% surviving patients, 54.28% had complete recovery of renal function, 12.85% partial recovery and 14.28% required chronic dialysis. In our study, all patients required dialysis at presentation, which was the inclusion criterion while only 55-70% of patients required dialysis in other studies as they have also included risk and injury groups of PAKI. Casablanca study reported complete recovery in 87.35% of their patients of PAKI.[19] The high incidence of patchy cortical necrosis in postobstetric cases is challenging clinical scenario. Studies have reported a very high incidence of cortical necrosis up to the tune of 24% in India.[826] A recent study reported cortical necrosis in 14.28% of cases. However, in a recent study from India, Prakash et al. reported that renal cortical necrosis following obstetrical complication decreased significantly; 4.7% in the 1990s to 0.5% of the total AKI cases, in the 2000s.[9] Postabortal PAKI leading to renal cortical necrosis is rare (1.5%) in western countries; however, it is still common in developing countries.[27]
The major limitation of the study is that it is a retrospective analysis and included only PAKI patients requiring dialysis. The PAKI patients in risk and injury groups were not included in the study as obstetrics facilities are not available at the institute and PAKI patients who do not require dialysis are not admitted. The major strength of the study is that the study highlights the high mortality associated with PAKI despite the advances in dialysis techniques and management of AKI in the present century primarily because of late referral in critically sick condition. The study population consisted of patients from one of the states with the highest maternal mortality in India.
Conclusions
Postabortal sepsis is the most common cause of PAKI. PAKI is associated with high maternal and fetal mortality. Oligoanuria, sepsis and CNS involvement at presentation is associated with greater risk of mortality in PAKI. The chance of renal function recovery becomes poor if no evidence of recovery is seen at 6 weeks; however, PAKI patients should be watched up to 6 months for dialysis independency state.
Source of Support: Nil
Conflict of Interest: None declared.
References
- Etiopathogenesis of acute renal failure in the tropics. Ann Natl Acad Med Sci (India) l. 987;;3:88-99.
- [Google Scholar]
- Renal cortical necrosis in pregnancy-related acute renal failure. J Indian Med Assoc. 1996;94:227-9.
- [Google Scholar]
- Decreasing incidence of renal cortical necrosis in patients with acute renal failure in developing countries: A single-centre experience of 22 years from Eastern India. Nephrol Dial Transplant. 2007;22:1213-7.
- [Google Scholar]
- Changes in frequency and etiology of acute renal failure in pregnancy (1980-1997) Ren Fail. 1998;20:513-7.
- [Google Scholar]
- An assessment of the RIFLE criteria for acute renal failure in hospitalized patients. Crit Care Med. 2006;34:1913-7.
- [Google Scholar]
- Challenges in diagnosis and treatment of acute kidney injury during pregnancy. Nephrourol Mon. 2012;4:340-4.
- [Google Scholar]
- Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest. 1992;101:1644-55.
- [Google Scholar]
- Mortality after acute renal failure: Models for prognostic stratification and risk adjustment. Kidney Int. 2006;70:1120-6.
- [Google Scholar]
- Pregnancy-related acute renal failure: A single-center experience. Indian J Nephrol. 2008;18:17-21.
- [Google Scholar]
- Changing trends in pregnancy related acute renal failure. J Obstet Gynecol India. 2002;52:36-8.
- [Google Scholar]
- Epidemiologic trend changes in acute renal failure - a tertiary center experience from South India. Ren Fail. 2006;28:405-10.
- [Google Scholar]
- Etiology and prognosis in 36 ARF cases related to pregnancy in central Anatolia. Eur J Gen Med. 2005;2:110-3.
- [Google Scholar]
- Obstetrical acute renal failure. Experience of the nephrology department, Central University Hospital Ibn Rochd, Casablanca. Nephrologie. 2001;22:29-31.
- [Google Scholar]
- Is pregnancy-related acute renal failure a disappearing clinical entity? Ren Fail. 1996;18:575-84.
- [Google Scholar]
- One-year renal outcome of pregnancy related kidney failure. J Pak Inst Med Sci. 2004;15:834-8.
- [Google Scholar]
- Acute renal failure of obstetrical origin during 1994 at one center. Ren Fail. 1996;18:681-3.
- [Google Scholar]
- Acute renal failure in pregnancy: One year observational study at Liaquat University Hospital, Hyderabad. J Pak Med Assoc. 2008;58:61-4.
- [Google Scholar]
- Spectrum of renal cortical necrosis in acute renal failure in eastern India. Postgrad Med J. 1995;71:208-10.
- [Google Scholar]
- Diagnostic procedures and long-term prognosis in bilateral renal cortical necrosis. Kidney Int. 1973;4:390-400.
- [Google Scholar]







