Translate this page into:
Spectrum of renal involvement in hematolymphoid neoplasms: Renal biopsy findings of 12 cases
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Spectrum of causes for renal dysfunction in patients with hematolymphoid malignancy (excluding plasma cell dyscrasia) is varied. A retrospective evaluation of “native” renal biopsies referred to our institute during the period from January 2010 to December 2013 revealed 12 cases. Age ranged between 7 and 69 (median 54.5) years. All patients were males. The neoplasms included non-Hodgkin lymphoma, chronic lymphocytic leukemia, acute lymphoblastic leukemia, Burkitt's lymphoma, intravascular lymphoma, Hodgkin lymphoma and chronic myeloid leukemia. Proteinuria was noted in 66% of the patients (nephrotic range in 5, subnephrotic range in 3). Renal insufficiency was noted in 100% patients. Malignancy-related kidney injury was noted in 75% of the cases. Renal histology showed lymphomatous infiltration (8), membranoproliferative glomerulonephritis (MPGN) (3), intracapillary monoclonal deposit disease (1) and intravascular lymphoma (1). Distribution of lymphomatous infiltration was diffuse in 50% and focal in 50%. We observed that renal dysfunction was predominantly a direct effect, that is, lymphomatous invasion. Paraneoplastic glomerulopathic changes occur in the form of MPGN. Proteinuria of >2 g/day correlated with glomerular disease.
Keywords
Hematolymphoid malignancy
intravascular lymphoma
lymphoma infiltration
paraneoplastic glomerulopathy
renal biopsy
Introduction
One of the reasons for seeking nephrology consultation by oncology department is malignancy-associated kidney impairment or chemotherapy-induced damage. Clinical manifestation of a subset of their patients, that is, hematolymphoid malignancy-related renal failure (other than plasma cell dyscrasia) is present in 1–2% of patients with infiltration of renal parenchyma.[1] The spectrum of renal disease association with hematolymphoid neoplasm is continuously expanding. Paraneoplastic glomerulopathies are increasingly recognized.[23] Most cases with renal function derangement respond to effective treatment of underlying neoplasm. The aim of this study was to compile clinical and histologic lesion of underlying malignancies, indication for biopsy, and characteristics of nephropathies.
Subjects and Methods
A retrospective evaluation of 7,509 “native” renal biopsies referred to our institute during the period from January 2010 to December 2013 revealed 12 cases of hematolymphoid neoplasms (excluding plasma cell dyscrasia) affecting kidney. Details of investigations and indication of renal biopsy were obtained from medical records and telephonic conversation with outside referral physician. Standard processing of renal biopsies included light microscopy (haematoxylin and eosin, periodic acid-Schiff [PAS], Masson's trichrome, periodic acid silver methenamine and congo red) and immunofluorescence (IF) (IgG, IgA, IgM, C3c, C1q, fibrin, kappa and lambda). Immune-mediated glomerular injury was defined as ≥2+ intensity staining on a scale of 0–4+ with any of the immunoglobulin/complements. Histology was assessed for hypercellularity, double contour of basement membranes, accentuation of lobules, rupture of capillary basement membranes and Bowman's capsule; tubular injury/chronicity; interstitial infiltrates (diffuse or focal) and vascular changes. Immunohistochemistry was performed using antibodies against CD20, CD3, kappa, lambda and Ki-67. CD34 staining was performed in 1 case.
Results
There were 12 patients aged between 7 and 69 years (median, 54.5 years). Surprisingly all patients were males. Hematolymphoid neoplasms include non-Hodgkin lymphoma (NHL), chronic lymphocytic leukemia (CLL), acute lymphoblastic leukemia, Burkitt's lymphoma (BL), intravascular lymphoma, Hodgkin lymphoma and chronic myeloid leukemia (CML). Clinical presentation, laboratory investigations, hematolymphoid pathology and duration between the diagnosis of neoplasm and renal derangement are shown in Table 1. Proteinuria was noted in 66% of patients (nephrotic [NP] range in 5, subnephrotic [SNP] range in 3). Renal insufficiency (RI) was noted in 100% patients. Serum creatinine ranged from 1.9 mg/dl to 11.5 mg/dl. Serology for serum protein electrophoresis (SPEP) was negative for M band, except for 1 case. Duration between detection of hematolymphoid neoplasm and renal dysfunction ranged from 3 months to 48 months in 11 cases. However, one patient was detected simultaneously to have renal failure and found to be renal intravascular lymphoma. Bone marrow examination in this case showed trilineage hypercellular marrow elements with foci of hemophagocytosis.

Histology
Lymphomatous infiltrates
Eight cases had a neoplastic lymphoplasmacytic infiltration in the interstitium, distributed diffusely in 4 (50%) [Figure 1] and patchy in another 4 cases. Nodular pattern of lymphoid infiltrates was noted in 2 cases [Figure 2]. Cells were small- to medium-sized with scant amount of cytoplasm, inconspicuous nucleolus. Mitotic figures were absent. Renal tubules were separated as result of lymphoid infiltrates. Immunostaining demonstrated predominance of CD20+/CD3− lymphoid infiltrates. Ki-67 labeling was low.

- (a) Diffuse leukemic infiltrates of B-acute lymphoblastic leukemias. (b) Lymphoblasts are moderate to large in size with irregular nuclear chromatin and scanty cytoplasm

- (a) Diffuse nodular aggregates of lymphoid infiltrates. (b) CD20- positive clonal nodular lymphoid infiltrates with negative CD3 (c) and low Ki-67 index (d). (e) Glomerulus shows heterogeneous mesangial nodule formation with occasional double-contoured basement membranes
Membranoproliferative glomerulonephritis (Cases 3)
Three cases had membranoproliferative glomerulonephritis (MPGN) pattern. Cellular proliferation and increase in mesangial matrix were heterogeneous from one glomerulus to another. Endocapillary hypercellularity and mesangial abnormality were more prominent than duplication of glomerular basement membranes, which appeared segmental [Figure 2]. IF showed granular deposits with C3 (2+) in the mesangial region globally [Figure 3]. Crescents and necrotizing lesion were not seen.

- (a) Glomerulus revealing global endocapillary proliferation with small lymphocytic infiltrates seen surrounding the glomerulus. (b) Predominant mesangial C3 granular deposits in tufts
Intravascular B-cell lymphoma (Case 1)
Large- to medium-sized immature lymphoid cells were seen predominantly in the lumen of peritubular capillaries. Cells were CD20+/CD3− with kappa light chain restriction [Figure 4]. CD34 highlighted the peritubular capillaries. There was no evidence of nodal enlargement either on clinical examination or computed tomography imaging of the whole body.
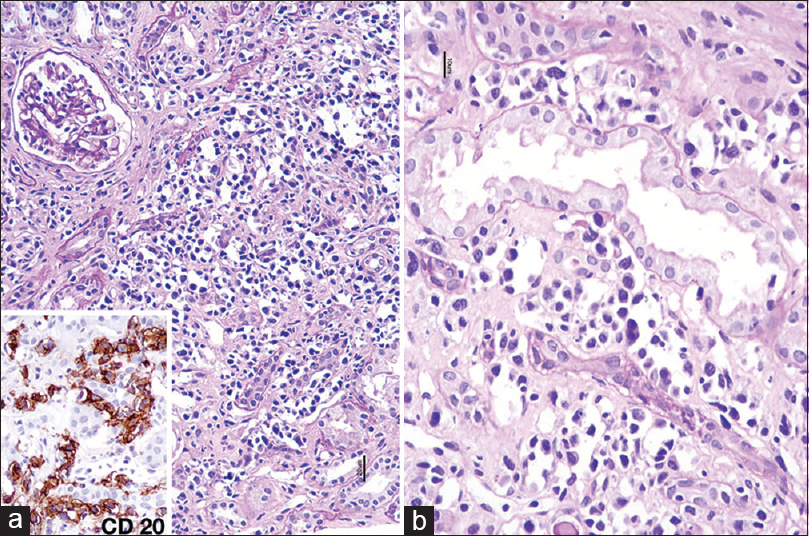
- (a) Medium- to large-sized monotonous lymphoid cells filling peritubular capillaries. (b) Some of the lymphoid cells are plasmacytoid with coarse chromatin. Inset shows positive staining with CD20
Intracapillary monoclonal deposit disease (1 case)
Two out of 11 glomeruli contained capillary thrombi that were negatively stained with PAS and trichrome stains. These thrombi were positive for IgM with kappa light chain restriction [Figure 5]. Other significant findings included moderate acute tubular injury and patchy interstitial lymphomatous infiltrates as mentioned in lymphomatous infiltrates. SPEP showed M band. Axillary lymph node biopsy had earlier revealed low-grade lymphoplasmacytic lymphoma.
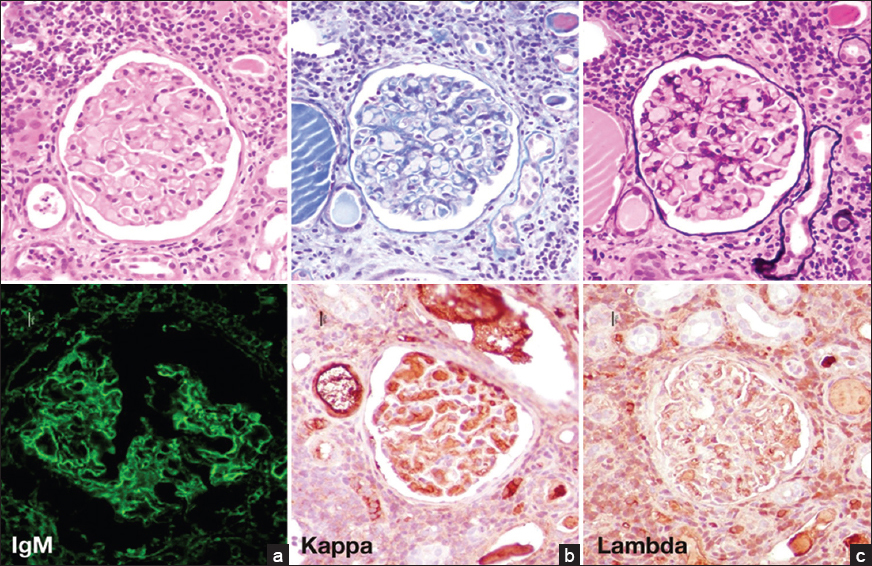
- Capillary lumen deposits are negatively stained with trichrome (upper mid) and PASM (upper right). They stain briskly with (a) IgM and (b) kappa light chain. (c) Lambda light chain is negative
Acute tubular necrosis
One case with BL had features of diffuse simplification of lining epithelium without any interstitial infiltrates.
Miscellaneous
These were especially seen in cases with Hodgkin lymphoma (2) and CML (1), where histology was not due to neoplasm, rather chronic diabetic nephropathy (DN), chronic interstitial nephritis (CIN) and focal segmental glomerulosclerosis (FSGS), respectively.
Discussion
Hematologic disorders invariably have detrimental effects on the renal system. A major group of hematologic disorder is hematolymphoid malignancies causing renal function derangement, with multiple mechanisms. Renal function derangement in hematolymphoid neoplasms can be attributed to pre-renal, intrinsic and post-renal causes. A handful of cases are reported in the form of single case reports from India at different time points, on lymphoma infiltration, intravascular lymphoma, and primary renal lymphoma causing renal dysfunction.[456789101112131415] We present here a case series of patients who have undergone renal biopsy in the evaluation of intrinsic causes of renal injury (i.e. lymphomatous infiltration, tubulointerstitial injury and paraneoplastic glomerulopathy).
Lymphomatous interstitial infiltration is observed in 8 cases (75%), as a diffuse process (50%) or patchy phenomenon (50%). Lymphomatous infiltration is hypothesized to cause renal dysfunction secondary to increased edema leading to increased pressure and compressing tubules as well as compromising blood flow with eventual acute tubular injury. All were found to be of B-cell lineage. We believe that lymphomas of B-cell phenotype are prone for renal involvement mainly because of the high prevalence among the hematolymphoid subtypes.[16] Few case reports are associated with T-cell neoplasms.[71718] Grade of NHL were low in 5, intermediate in 2 and high grade in 2 cases. Our series is in conjunction with literature in that low-grade lymphomas are more common to affect glomerular compartment versus nonglomerular compartment in high-grade lymphomas. RI was the presentation in all of these cases. Richmond et al. described that renal involvement is associated with metastasis to other organs, including heart, lungs and gastrointestinal tract in an autopsy material of 690 NHL cases.[14]
Paraneoplastic glomerulopathy may precede, coexist or even follow the diagnosis of lymphoma up to several years.[151920] All of our cases except one presented 3 months postdiagnosis of nodal lymphoma to 13 months postchemotherapy. Glomerular diseases that are well described include MCNS and membranous glomerulonephritis (MGN) especially following Hodgkin lymphoma. Rarely, immunotactoid glomerulopathy, cryoglobulinemic MPGN, amyloidosis, monoclonal immunoglobulin deposit disease and necrotizing pauci-immune crescentic glomerulonephritis have been described.[3151920212223] Autoimmune mechanisms and T-lymphocyte dysfunction are implicated in the pathogenesis.[20] In 5 patients of our series with NP range proteinuria, 3 had MPGN, 1 had FSGS and another 1 had DN. In 3 patients with SNP range proteinuria, proteinuria was ascertained to tubular nature in two of them and one associated with glomerular intracapillary monoclonal deposits. Latter patient had monoclonal band in serum. Audard et al. have described glomerular lesions in IgM-secreting hematologic lesions, presenting with RI with NP range/or SNP range proteinuria.[24] Two patients with Hodgkin disease underwent renal biopsy. One of them had NP range proteinuria attributed to co-morbidity of long-standing DN and another case with RI was attributed to CIN. In the absence of co-morbidities, we noticed that clinicopathologic correlation of NP range proteinuria is more likely to be MPGN. The latter group had C3 deposits alone in the IF, which is in accordance to the cases described by Sethi and Fervenza.[25] Association of CLL and MPGN was reviewed by Da’as et al.[22] In their review of 42 cases, majority of patients had NP range proteinuria with the most common glomerular lesion of MPGN (35.7%) and followed by MGN.[2122] We noticed focal segmental sclerosis in one case of CML. However, duration of gap between disease onset and renal biopsy is short to confirmatively link cause and effect. The mean duration between malignancy and renal biopsy diagnosis was 7.2 years in a review of 11 cases by Said et al.[26]
Case 8 had a peculiar distribution of high-grade lymphoma with cells occupying peritubular capillary lumen space staining for B-cell lineage. Intravascular B-cell lymphoma (IVBCL) was diagnosed after exclusion of nodal enlargement through radiologic assessment. IVBCL, an aggressive type, was defined in 2008 by WHO as extranodal large B-cell lymphoma where growth of lymphoma cells is restricted to lumina of vessels, especially capillaries involving renal system, skin and central nervous system.[1627] Most often, diagnosis is obtained at autopsy without any clue during life.[4]
In summary, this is the largest series reported from India of hematolymphoid neoplasms (other than plasma cell dyscrasia [PCD]) affecting intrinsic/parenchymal renal injury. Renal dysfunction is predominantly due to direct effect of hematolymphoid neoplasm (other than PCD), contrary to predominant indirect effects of PCD (unpublished personal files). Paraneoplastic glomerulopathic changes in the form of MPGN are common in long-standing cases of low-grade NHL and CLL; manifested clinically as proteinuria and renal failure. Proteinuria of >2 g/day correlated with glomerular disease. Multiple pathologies could be seen simultaneously. Limitation of this study is that it's observational and retrospective, lacking information on therapeutic details and also ultrastructure details.
Acknowledgment
Project team wishes to thank all referring nephrologists for providing the clinical results, and renal biopsy material. We sincerely thank Mrs. Thulasi Kumari, Mrs. Hema Nagaraj and Mr. Nagaraj for their outstanding technical support in Histopathology section.
Source of Support: Nil
Conflict of Interest: None declared.
References
- Acute renal failure due to lymphomatous infiltration of the kidneys. J Am Soc Nephrol. 1997;8:1348-54.
- [Google Scholar]
- Glomerular diseases seen with cancer and chemotherapy: A narrative review. Kidney Int. 2013;84:34-44.
- [Google Scholar]
- Glomerular diseases associated with hematopoietic neoplasms: An expanding spectrum. Kidney Int. 2011;80:701-3.
- [Google Scholar]
- A case with paraplegia, urinary tract infection and renal failure. Indian J Nephrol. 2007;17:80-86.
- [Google Scholar]
- An unusual case of bilateral renal enlargement due to primary renal lymphoma. Indian J Nephrol. 2011;21:56-8.
- [Google Scholar]
- Primary renal lymphoma mimicking renal cell carcinoma. Indian J Urol. 2010;26:441-3.
- [Google Scholar]
- Paediatric T cell lymphoma with nephrotic syndrome: A rare association. Indian J Hematol Blood Transfus. 2014;30:45-7.
- [Google Scholar]
- Renal enlargement as primary presentation of acute lymphoblastic leukaemia. Indian J Cancer. 2002;39:154-6.
- [Google Scholar]
- Non-Hodgkins lymphoma in a child presenting as nephromegaly and acute renal failure. Indian Pediatr. 2001;38:407-10.
- [Google Scholar]
- Acute renal failure due to leukaemic infiltration of kidneys. J Assoc Physicians India. 1990;38:284-6.
- [Google Scholar]
- Acute renal failure – An unusual presentation of non-Hodgkin's lymphoma (an autopsy report) J Assoc Physicians India. 1985;33:801-2.
- [Google Scholar]
- Renal involvement in hematological malignancies. J Assoc Physicians India. 1985;33:565-8.
- [Google Scholar]
- Acute renal failure due to lymphomatous infiltration of kidneys (a case report) J Assoc Physicians India. 1981;29:675-7.
- [Google Scholar]
- Minimal change nephrotic syndrome and classical Hodgkin's lymphoma: Report of 21 cases and review of the literature. Kidney Int. 2006;69:2251-60.
- [Google Scholar]
- Lymphomas diagnosed by percutaneous kidney biopsy. Am J Kidney Dis. 2003;42:960-71.
- [Google Scholar]
- Primary bilateral T-cell renal lymphoma presenting with sudden loss of renal function. Nephrol Dial Transplant. 2001;16:1487-9.
- [Google Scholar]
- A 30-month-old child with acute renal failure due to primary renal cytotoxic T-cell lymphoma. Am J Surg Pathol. 2010;34:1066-70.
- [Google Scholar]
- Onco-nephrology: Glomerular diseases with cancer. Clin J Am Soc Nephrol. 2012;7:1701-12.
- [Google Scholar]
- Paraneoplastic glomerulopathies: New insights into an old entity. Kidney Int. 1999;56:355-77.
- [Google Scholar]
- Kidney involvement and renal manifestations in non-Hodgkin's lymphoma and lymphocytic leukemia: A retrospective study in 700 patients. Eur J Haematol. 2001;67:158-64.
- [Google Scholar]
- Acute renal failure in a patient with acute lymphoblastic leukemia: A rare cause. Saudi J Kidney Dis Transpl. 2013;24:93-6.
- [Google Scholar]
- Renal lesions associated with IgM-secreting monoclonal proliferations: Revisiting the disease spectrum. Clin J Am Soc Nephrol. 2008;3:1339-49.
- [Google Scholar]
- Membranoproliferative glomerulonephritis: Pathogenetic heterogeneity and proposal for a new classification. Semin Nephrol. 2011;31:341-8.
- [Google Scholar]







