Translate this page into:
Causes of death in renal transplant recipients with functioning allograft
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
The survival of transplant recipients is significantly lower than age-matched controls in the general population. The aim of this study was to analyze the trends in mortality of renal allograft recipients at our centre. We retrospectively analyzed data from all patients who were transplanted between October 1988 and June 2010 and were followed at our center. Patients were considered to have death with graft function (DWGF) if death was not preceded by return to dialysis or re-transplantation. The study included 98 renal allograft recipients (male : female – 7.99 : 1). The mean recipient and donor ages were 35.06 ± 11.84 (range: 15–69) and 41.17 ± 10.44 (range: 22–60) years, respectively. Basic kidney diseases were CGN (chronic glomerulonephritis) (60.20%), CIN (chronic interstitial nephritis) (15.31%), DN (diabetic nephropathy) (8.16%), ADPKD (autosomal dominant polycystic kidney disease) (2.04%) and others (14.29%). They were followed up for a mean 79.91 ± 60.05 patient-months. Mortality occurred in 25 (25.51%) patients (male : female – 4 : 1). Causes of death were sepsis/infection (36%), coronary artery disease (28%), CVA (8%), failed graft (4%), and rest unknown (24%). DWGF was 88% of total death and contributed to 78.57% of total graft loss. Overall patient survival at 1, 5, 10, and 15 years were 90.8%, 80.2%, 65.6%, and 59.1%, respectively (Kaplan–Meier analysis). Those who died exhibited significant differences in recipient's age (median 40 years vs 31 years, P=0.007), pretransplantation hypertension (HTN) (100% vs 65.75%, P<0.001), post-transplant infection (76% vs 42.47%, P=0.005), coronary artery disease (28% vs 1.37%, P<0.001), and serum creatinine at last follow up (median 2.3mg/dL vs 1.56mg/dL, P=0.003). Cardiovascular disease, in addition to infection, is an important cause of death during the first 15 years following renal transplantation even in nondiabetic recipients. Death with functioning graft is of concern.
Keywords
CVD
death with graft function
infection
mortality
renal transplantation
Introduction
Renal replacement therapy (RRT) of choice for patients with end-stage renal disease (ESRD) is renal transplantation as it gives better survival, quality of life, and cost effectiveness.[1–5] Although renal transplantation confers a robust survival advantage over dialysis treatment for patients with ESRD, the survival of transplant recipients is significantly lower than age-matched controls in the general population. The relatively higher mortality in renal transplant recipients is related to co-morbid medical illnesses, pretransplant dialysis treatment, and factors uniquely related to transplantation, including immunosuppression and other drug effects. Death with graft function (DWGF) has been reported in 9% to 30% of patients, thus accounting for a substantial fraction of graft loss.[6–9] Infection was the leading cause of death in renal transplant recipients between 1970s to mid-1980s.[10–15] However, since then there has been change in the practice pattern with newer immunosuppressive protocols, improved surgical techniques and transplantation in older and sicker patients.[1617] Thus, the risks and determinants of mortality in the renal transplant recipients need to be reassessed. There is limited data from India regarding mortality in adult population of renal allograft recipients. The aim of this study was to analyze the trends of mortality in renal allograft recipients observed at our centre.
Materials and Methods
We retrospectively analyzed data from all patients followed-up at our center who were transplanted between October 1988 and June 2010. Patients were considered to have died with the graft function if death was not preceded by return to dialysis or re-transplantation. Statistical analysis was done using Sigmastat 3.5 software. P value of <0.05 was taken as the point of significance.
Results
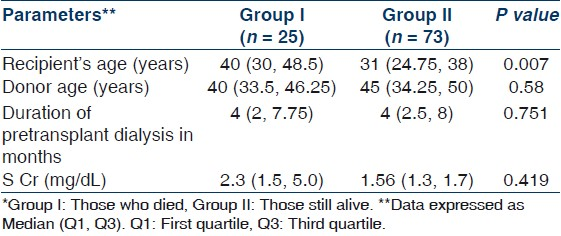
The study included 98 living donor renal allograft recipients (male : female – 7.99 : 1). The mean recipient and donor ages were 35.06±11.84 (range: 15–69) years, and 41.17±10.44 (range: 22–60) years, respectively. Basic kidney diseases were chronic glomerulonephritis (60.20%), chronic tubulointerstitial nephritis (15.31%), diabetic nephropathy (8.16%), autosomal dominant polycystic kidney disease (2.04%), and others (14.29%). The patients were followed for a mean 79.91±60.05 patient-months and their demographic profile is given in Table 1.
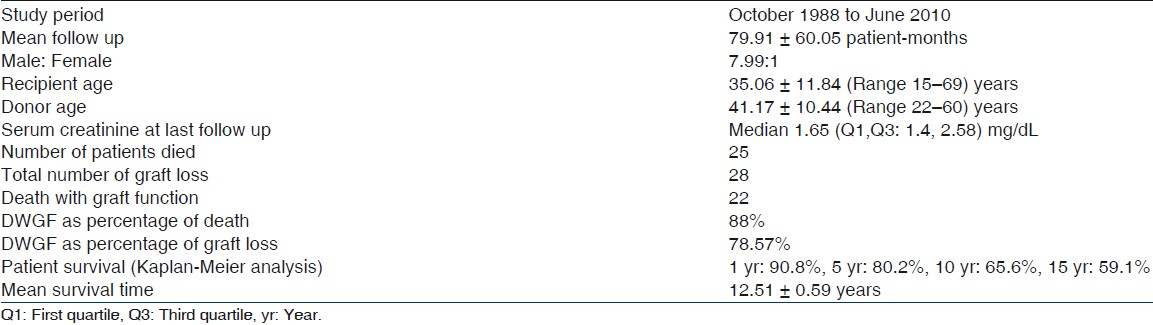

Mortality occurred in 25 (25.51%) patients (M: F – 4: 1). Causes of death were sepsis/infection (36%), coronary artery disease (CAD) (28%), cerebrovascular accident (CVA) (8%), failed graft (4%) and the rest unknown (24%). The infections leading to death were bacterial pneumonia (n=3), bacterial urinary tract infection (n=1), tuberculosis (n=2), systemic candidiasis (n=1), and sepsis with unknown primary site of infection (n=2). All seven patients who died of CAD had clinical and ECG evidence of acute coronary syndrome. Cardiovascular diseases (CVD ie, CAD and CVA combined) and sepsis/infection accounted for 44.44% and 33.33% of deaths in the first year. Sepsis/infection continued to be the major cause of death (66.67%) 1 to 5 years post-transplant. CAD was the predominant cause of death in 5 to 10 years post-transplant (66.67%). All deaths due to sepsis/infection occurred within 5 years of post-transplant whereas more than half of deaths due to CAD occurred after 5 years of transplantation. Patient survival by Kaplan–Meier analysis [Figure 1] was 90.8% at 1 year, 80.2% at 5 years, 65.6% at 10 years, and 59.1% at 15 years with mean survival time of 12.5±0.59 years. Recipient age strongly predicted the chance of survival when multivariate logistic regression analysis was done taking duration of pretransplant dialysis, recipient age, donor age, and post-transplantation follow-up period.
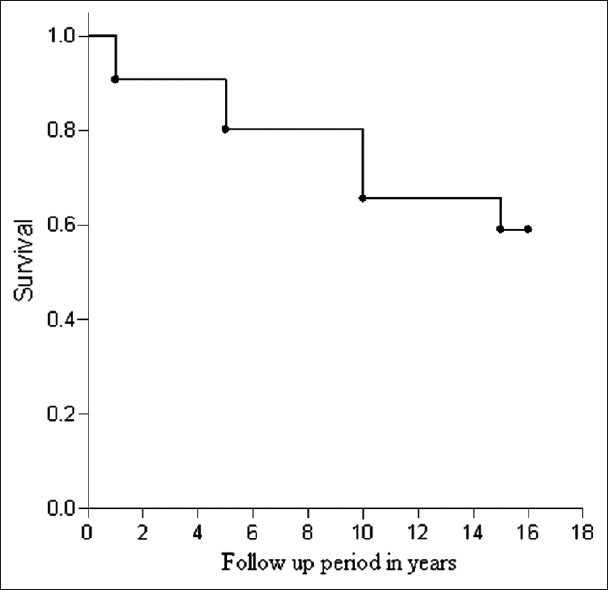
- Kaplan–Meier survival analysis
Demographic and clinical parameters comparing those who died with those still alive are given in Tables 2 and 3, respectively. A number of factors were identified as predisposing to death when the group with mortality was compared to those still alive. These were recipient age (median 40 years vs 31 years, P=0.007), pretransplantation hypertension (HTN) (100% vs 65.75%, P<0.001), post-transplant infection (76% vs 42.47%, P=0.005), coronary artery disease (28% vs 1.37%, P<0.001) and level of the graft function as judged by serum creatinine at last follow-up (median 2.3 mg/dL vs 1.56 mg/dL, P=0.003). Recipient's gender, pretransplant dialysis duration, basic kidney disease, immunosuppression regime, number of acute rejection episodes, presence of chronic allograft nephropathy and donor age, gender and relation to the recipient, were not significantly different between the two groups. Most patients were on triple immunosuppressive regimen consisting of cyclosporine, azathioprine, and prednisolone [Table 3].
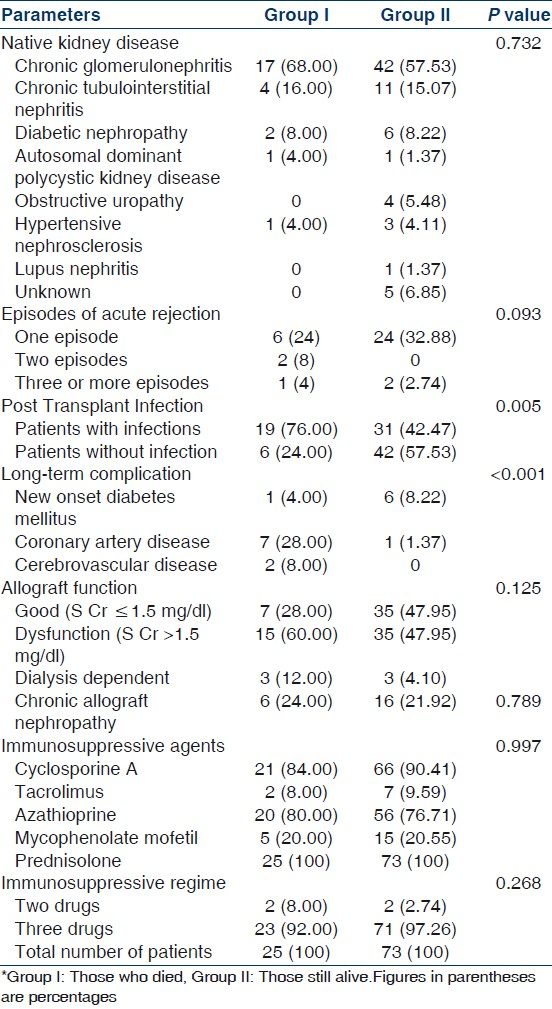
The graft function was good (S.Cr ≤ 1.5 mg/dL) in 7(28%) cases at the time of death. Serum creatinine range was >1.5 to ≤ 3 mg/dL in 40% cases and ≥3mg/dL in 32% cases at the time of death. Thus, majority (68%) of patients had relatively good graft function (S.Cr.<3) at the time of death while only three (12%) patients were dialysis dependent. Among those still alive (n=73) three patients are currently dialysis dependent. Thus, DWGF (n=22) was 88% of total death (n=25) and contributed to 78.57% of total graft loss (n=28). Causes of DWGF were sepsis/infection (40.91%), CVD (36.36%), and unknown (22.73%). Among patients with DWGF, those died within 1 year were compared to those died >1 year post-transplantation. Although recipient's age was significantly different (34.86±8.47 vs 44.93±10.17 years, P=0.034) their gender, cause of ESRD, post-transplant complications such as acute rejection, infection, NODM, and causes of death were not different.
Discussion
In early 1980s, graft rejection and infection were the major challenges in transplant patients.[10–15] However, episodes of rejection decreased with the use of newer immunosupressive agents and balanced immunosupressive protocols. There have been tremendous advances in general medical management both before and after renal transplantation over the past decades.[518] As a result, both patient and graft survival have improved.[18] The greatest decrement in both mortality and graft failure occurred after 1985, corresponding to the widespread adoption of cyclosporine therapy. As the patient survival improved, the trends in mortality have changed with cardiovascular causes being more common than infections especially in western countries.[19–22] Future risk of mortality from CVD has been reported to be most pronounced in diabetics in whom the adjusted CVD death rate was two-fold higher than any other groups.[2324]
As infectious diseases are high in our country similar to other developing countries, we analyzed our records to see the trends of mortality in our transplant recipients. We found equal (36%) prevalence of infection and cardiovascular disease in our patients. High prevalence of death due to cardiovascular disease (coronary artery disease: 28% and cerebrovascular disease: 8%) in our population was seen despite the fact that none had clinically evident ischemic heart disease before transplantation and most transplant recipients had basic disease of CGN and not diabetic nephropathy in contrast to the western literature. Sepsis was reported as a major cause of patient death in pediatric renal transplant recipients from our country.[25] This is in line with the rarity of cardiovascular disease in pediatric transplant population. In a study from the United States, cardiovascular disease was the most common cause of mortality (36.1%) followed by infections/sepsis (17.6%).[23] Another study reported cardiovascular disease and infections as major causes of death (31.4% and 31.1%, respectively in 1970s whereas 51.1% and 21.6%, respectively in 1980s).[24] Thus, the incidence of cardiovascular events causing mortality in our patient population was similar to other western studies. However, infections especially bacterial sepsis and systemic fungal infection were still major causes of mortality in renal transplant recipients in our country. Overall survival of renal transplant recipients in our study was comparable to other studies from India.[26]
Death with functioning graft was seen in 88% of our patients as compared to only 9% to 38% as reported by others.[6–9182327] Ojo et al. studied 86 502 renal transplant recipients more than 18 years old who were transplanted between 1988 and 1997.[18] Out of 18 482 deaths in their study 38% (n=7040) were DWGF which also accounted for 42.5% of graft loss. The adjusted rate of DWGF was 4.6, 0.8, 2.2, and 1.4 deaths per 1000 person-years for cardiovascular disease, stroke, infections, and malignancy, respectively. However, the risk of DWGF decreased by 67% (RR=0.33, P<0.001) between 1988 and 1997. Recently Kahwaji et al. studied cause of DWGF among renal transplant recipients in an integrated healthcare system and found a low rate of DWGF because of CVD (24%) as compared to that found by Ojo et al. (36%), while the DWGF due to infection (16%) and malignancy (12%) remained almost similar in both studies.[1827] Kahwaji et al. postulated that the low rate of DWGF due to CVD could be due to better coordinated care within an integrated healthcare system.[27] Overall, lower hemoglobin, uncontrolled blood pressure, and lower albumin levels were associated with DWGF.[27] CVD has been reported to be the most common cause of DWGF ranging from 36% to 55%.[1827–30] Risk factors for DWGF and CVD in renal allograft recipients were found to be new-onset-diabetes after transplant, hypertension, hyperlipidemia, anemia, hypoalbuminemia, tobacco use, obesity, lack of exercise, and immunosuppressive agents.[1827–30] We found very high rate of infection (40.91%) and CVD (36.36%) as causes of DWGF. Moreover, out of 22.73% of DWGF where cause was not known, most deaths occurred in home and a cardiac cause could not be ruled out. The high incidence of DWGF in our study may be due to poor hygiene, ignorance, and late arrival of patients to hospital with bacterial infection and sepsis as well as lesser attention to reduce cardiovascular risk factors leading to high incidence of fatal cardiovascular events. During the study period, we did not have facility for coronary angiography and intervention in our centre. However, patients who died of acute coronary syndrome presented quite late in the natural history of their myocardial infarction (MI) precluding any coronary artery interventions even if we had those facilities. They all had very bad cardiac prognosis in view of massive MI and cardiogenic shock at presentation. This is a major obstacle in caring for transplant recipients, a substantial proportion of whom develop and eventually die of cardiovascular disease. Therefore, good transplantation practice asks for a good cardiology team incorporated in the transplantation program.
Conclusion
Though patient survival was good (mean 12.5±0.59 years) DWGF was very high (88%) in our renal transplant recipients. CVD was a major cause of mortality in both the early (first year) and late (>5 years) post-transplant periods. High prevalence of CVD in transplant recipients of even nondiabetic population without clinically evident pretransplant ischemic heart disease calls for an urgent attention to prevention of CVD in all recipients. Attention to cardiovascular risk factors along with prevention and prompt treatment of infection would offer the greatest potential to improve the chance of living longer with functioning graft.
Source of Support: Nil
Conflict of Interest: None to declare.
References
- Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med. 1999;341:1725-30.
- [Google Scholar]
- A study of the quality of life and cost-utility of renal transplantation. Kidney Int. 1996;50:235-42.
- [Google Scholar]
- The quality of life in renal transplantation — a prospective study. Transplantation. 1992;54:656-60.
- [Google Scholar]
- Comparison of treatment costs between dialysis and transplantation. Semin Nephrol. 1992;12:284-9.
- [Google Scholar]
- Ischemic heart disease-major cause of death and graft loss after renal transplantation in Scandinavia. Transplantation. 1995;60:451-7.
- [Google Scholar]
- Patient death renal transplantation-An analysis of its role in graft outcome. Transplantation. 1996;61:1479-83.
- [Google Scholar]
- Half-life and risk factors for kidney transplant outcome: Importance of death with function. Transplantation. 1993;55:757-61.
- [Google Scholar]
- Kidney transplant recipients who die with functioning grafts: Serum creatinine level and cause of death. Transplantation. 1996;62:1029-30.
- [Google Scholar]
- Causes of death after renal transplantation: A long-term follow-up study. Transplant Proc. 1994;26:2017-8.
- [Google Scholar]
- Causes of early or late patient death after living donor renal transplantation. Transplant Proc. 1994;26:2019-20.
- [Google Scholar]
- Changes in causes of death after renal transplantation, 1966 to 1987. Am J Kidney Dis. 1991;27:512-8.
- [Google Scholar]
- Long term morbidity and mortality after kidney transplantation. Scand J Urol Nephrol. 1992;26:397-401.
- [Google Scholar]
- Causes of death in kidney transplant recipients: 1970 to present. Transplant Proc. 1989;21:2168-70.
- [Google Scholar]
- The UNOS Scientific Renal Transplant Registry: United Network for Organ Sharing. Clin Transpl 1994:1-18.
- [Google Scholar]
- US Renal Data System. 1999 Annual Data Report. 1999; Bethesda, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases
- Long-term survival in renal transplant recipients with graft function. Kidney Int. 2000;57:307-13.
- [Google Scholar]
- Causes of death after renal transplantation. Nephrol Dial Transplant. 2001;16:1545-9.
- [Google Scholar]
- Mortality after kidney transplant failure: The impact of non-immunologic factors. Kidney Int. 2002;62:1875-83.
- [Google Scholar]
- Death with functioning graft in living donor kidney transplantation: Analysis of risk factors. Am J Nephrol. 2003;23:186-93.
- [Google Scholar]
- Trends in mortality and graft failure for renal transplant patients. CMAJ. 2002;167:137-42.
- [Google Scholar]
- Progress in renal transplantation: A single center study of 3359 patients over 25 years. Ann Surg. 1995;221:466-8.
- [Google Scholar]
- Causes of renal allograft loss. Progress in the 1980s, challenges for the 1990s. Ann Surg. 1991;214:679-88.
- [Google Scholar]
- Pediatric renal transplantation-A single centre experience of 15 yr from India. Paediatr Transplant. 2007;11:844-9.
- [Google Scholar]
- Evolution of renal transplantation in India over the last four decades. NDT Plus. 2010;3:203-7.
- [Google Scholar]
- Cause of death with graft function among renal transplant recipients in an integrated healthcare system. Transplantation. 2011;91:225-30.
- [Google Scholar]
- Cardiovascular disease after renal transplantation. J Am Soc Nephrol. 1996;7:158-65.
- [Google Scholar]
- Risk factors and management of post-tranplantation cardiovascular disease. BioDrugs. 2001;15:261-72.
- [Google Scholar]
- How to decrease cardiovascular mortality in renal transplant recipients. Transplant Proc. 2006;38:2887-92.
- [Google Scholar]







