Translate this page into:
Gelatin-thrombin hemostatic matrix injection to salvage refractory post-renal graft biopsy bleed
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Post-renal biopsy bleeding refractory to angioembolization usually requires graft nephrectomy as a life-saving measure. Gelatin-thrombin hemostatic matrix injection in the needle tract is a novel attempt to control bleeding in such cases and to salvage the allograft. We hereby describe two cases of post-graft biopsy bleed. Both these patients continued to bleed even after angioembolization. They were shifted to the operating room upon developing hypotension, having received multiple blood transfusions with the intention of performing graft nephrectomy to save their lives. However, bleeding was successfully controlled by using Gelatin-thrombin hemostatic matrix injection in the biopsy needle tract. Patients improved hemodynamically after the procedure. Graft function returned to normal in both the cases. At an average follow-up of 10.4 months, both the patients have shown stable graft functions.
Keywords
Hematuria
hemostatic matrix
renal biopsy
tissue sealant
Introduction
Renal biopsy is indicated to evaluate graft dysfunction following renal transplant. Bleeding is a major complication. However, post-renal biopsy bleeding is becoming infrequent with use of small-gauze bioptic gun.[1] Majority of the cases respond to conservative measures like bed rest and volume replacement. Those cases not responding to conservative measures may require selective renal angioembolization for the control of bleeding.[2] Rarely, even angioembolization fails and graft nephrectomy may be deemed necessary as a life-saving measure. Experience with hemostatic agents has shown that they are successful in controlling parenchymal bleed following solid organ superficial injuries.[3] Based on this information, we used FloSeal® hemostatic matrix to control bleeding following post-transplant graft biopsy in two cases.
Case Reports
Patient 1
A 47-year-old man received a renal allograft from his wife in December 2010 using prednisolone, tacrolimus, and mycophenolate mofetil, without any induction. In the immediate post-transplant period, his urine output was just 30 ml. Graft Doppler study showed reversal of diastolic flow in renal artery at hilum, segmental, and interlobar arteries and loss of diastolic flow in arcuate arteries. The patient was dialyzed. The next day, his total urine output was 60 ml and serum creatinine level was 3.6 mg/dl. He received another hemodialysis and underwent graft biopsy. Biopsy was unremarkable. There was no evidence of rejection or calcineurin inhibitors (CNI) toxicity. His creatinine showed a steady rise over the next few days to 7.7 mg/dl. His tacrolimus levels (C0) on Post-operative days four and seven were 7.4 ng/ml and 17.1 ng/ml, respectively, and tacrolimus dose adjustment was done accordingly. After ensuring a normal coagulation profile, a repeat biopsy was done on ninth post-transplant day using 18-gauge automated gun under real-time ultrasound guidance. Post-biopsy, the patient had progressive abdominal distension and drop in his hematocrit. Ultrasonography (USG) disclosed a large upper polar hematoma of approximately 650 ml. He developed hypotension and a total of 17 units of blood transfusions were given. This did not help, so emergency angiographic embolization was attempted. Angiography revealed an upper polar arterio-venous fistula for which the metallic clips were deployed. Even after this, he continued to bleed necessitating exploration. Having obtained the consent for graft nephrectomy, he was taken for exploration. Under general anesthesia, graft kidney was approached by opening the previous incision. On exploration, there was a large perinephric hematoma at the upper pole, which was evacuated and biopsy needle tract was identified. There was continuous bleeding from the tract, which continued even after applying local pressure. Hemostatic sutures also failed to stop the bleeding. So, 5 ml of Gelatin-thrombin hemostatic matrix was prepared as per the manufacturer's instructions. It was injected in the biopsy needle tract using 20 G intravenous cannula [Figure 1]. The bleeding stopped within a few minutes. Patient was hemodynamically stable and did not require any more transfusions after the exploration. Graft biopsy revealed features of ATN. He required four more sessions of hemodialysis after this. He started passing urine 16 days after the transplantation. The creatinine levels started declining and reached a nadir level of 1.1 mg/dl, four weeks after the transplant. He was discharged in a stable condition. He was last followed-up in Jan 2012 and maintained a stable graft function and well-being.
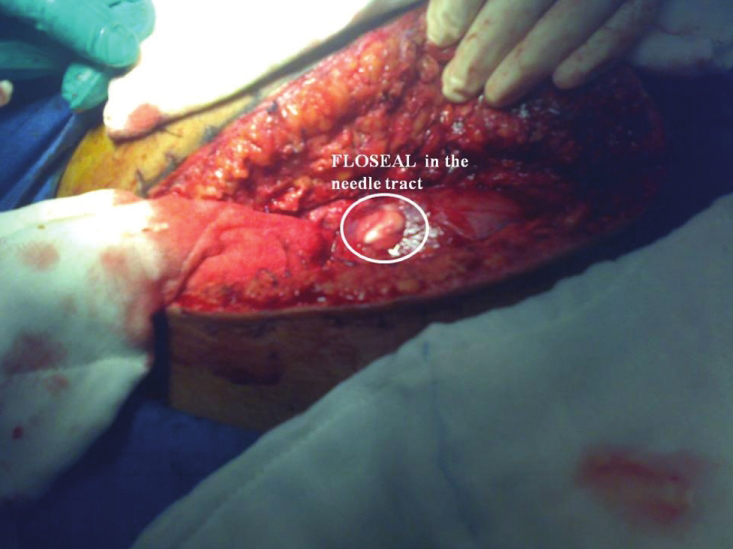
- Intraoperative photograph showing hemostatic matrix injected in the needle tract
Patient 2
A 41-year-old gentleman underwent renal transplant with his wife as the donor on 17th July 2011. He received basiliximab as induction and maintained on triple immunosuppression (prednisolone, tacrolimus, and mycophenolate mofetil). He continued to have good urine output through fourth post-operative day and his creatinine declined to 1.7 mg/dl. His tacrolimus levels (C0) on days two and five were 7.8 ng/ml and 9.3 ng/ml respectively. On fifth post-operative day, his serum creatinine level increased to 2.2 mg/dl with a decline in urine output. Laboratory investigations revealed hemoglobin of 9.6 mg/dl, a total count of 7100/mm2, a normal platelet count, coagulation and electrolyte profiles. Graft Doppler showed high resistive indices throughout the arterial tree beginning from renal artery at hilum. On sixth post-operative day, the creatinine rose to 2.6 mg/dl. USG-guided biopsy was done from the upper pole of the graft. Post-biopsy, he developed hematuria, which was initially managed with bed-rest, hydration, and other conservative measures. In the evening, his hemoglobin was found to be 7.2 mg/dl (a drop of 2.7 mg/dl in 8 h). He received two units of blood transfusions. He continued to have hematuria and developed hypotension. Repeat hemoglobin level after two units of transfusion was 6.9 mg/dl. He underwent angiography and transarterial embolization of upper polar pseudoaneurysm using metallic coils was attempted. In spite of this, his hematuria did not subside and there was a further drop in hematocrit. He was explored on the morning of 24th July. By this time, he had received five units of blood. Under general anesthesia, graft was approached by opening the previous incision. There was a small hematoma at the upper pole. After evacuating hematoma, a 2-cm superficial laceration apart from the tract site bleeding was identified. Attempts to close the laceration using prolene sutures in the capsule failed as the sutures cut through the edematous graft. Based on our previous successful experience with Gelatin-thrombin hemostatic matrix, we decided to use it in this case also. A total of 5 ml of the sealant was injected into the tract, in a manner similar to the previous case, and an additional 5 ml was used over the laceration site. In addition, the laceration site was covered with Surgicel. Bleeding was successfully controlled in this case as well. The patient became hemodynamically stable and his graft function improved after receiving anti-rejection therapy as his biopsy revealed C4d-negative acute cellular rejection (Banff 1A). He was discharged after two weeks with a serum creatinine level of 1.2 mg/dl. This patient has been on regular follow-up. He was admitted in April 2012 with culture-positive urinary tract infection with transient graft dysfunction.
Discussion
Like every invasive procedure, renal biopsy is fraught with potential complications. However, with the introduction of automated bioptic guns and real-time ultrasound guidance, the risk of complications has been dramatically reduced. Atwell et al. has reported a 6-7% incidence of bleeding after 15,181 percutaneous biopsies.[4] About one in 20 patients will notice mild self-limiting hematuria lasting for a few hours. About one in 200 will require a blood transfusion. About one in a 1000 patients will require an angioembolization or exploration.[4] Gainja et al. in their review of 142 percutaneous renal biopsies (seventy-three allografts and sixty-nine native kidneys) discovered that incidence of gross hematuria was more than double following allograft biopsies (9.9%) as compared to native-kidney biopsies. Even the serious complications (hematoma, hemoperitoneum and AV fistula) were more common following graft biopsies.[5]
Other complications include pain lasting for more than 12 h (4%), a palpable hematoma (1%), infection (0.2%), and death (0.2%).[6]
Majority of these complications have no consequences as such and percutaneous needle biopsy is a safe procedure. The safety of this procedure has been very well established in various studies. Benfield et al.[7] assessed the safety of kidney biopsy in pediatric kidney transplantation and they concluded that percutaneous renal biopsies can be safely performed in pediatric patients with minimal risks. The tissue, thus obtained, is instrumental in the care of these patients.
Majority of the bleeding episodes respond to conservative management, e.g. bed rest, hydration, and transfusion. Patients presenting with active bleeding and persistent hemodynamic instability in spite of conservative management, require immediate attention. First line of management includes super selective angioembolization. If embolization is not successful, exploration usually ends up with partial or total nephrectomy.[28] Performing this kind of emergent surgery requires a high level of technical expertise, especially in transplanted kidneys.
A review of the literature reveals success rates of embolization between 85% and 100%.[29] Hagiwara et al., believe that transarterial embolization of the culprit lesion, diagnosed on angiography, should be the first line of treatment in cases of renal arterial bleeding, whenever the clinical situation allows.[10] These authors postulate that super- selective embolization reduces the extent of the initial ischemic area and offers a rapid, precise, and effective treatment, allowing the highest possible level of preservation of renal function. Without arteriography, the attempts to stabilize such patients are unlikely to be successful, and emergency laparotomy and possible nephrectomy become the only option.[10]
Recently, several methods have been proposed to reduce post-biopsy bleeding in the abdominal solid organs.[11–16] These methods include plugging the biopsy tract using a coil,[11] fibrin sealants,[12] hemostatic agent such as an absorbable gelatin sponge,[15] or a Histoacryl – Lipiodol mixture,[16] and even the application of radiofrequency energy to occlude the biopsy tract.[17] Each of these techniques has been described as an effective post-biopsy bleeding reduction method. Noller et al.[18] reported no hemorrhagic complications in 10 consecutive renal units treated with fibrin sealant-assisted tubeless percutaneous nephrolithotomy (PCNL). The instillation of 2-3 ml of fibrin sealant into the parenchymal defect is performed as the sheath is removed at the conclusion of PCNL in lieu of nephrostomy drainage. In 1989, Kram et al.[19] first reported fibrin sealant use in 14 patients who presented with traumatic renal injuries. Paulson et al., described use of fibrin sealant injection into needle tract of post-liver biopsy bleeding to reduce post procedural bleeding in swine.[3]
Based on these studies, we used FloSeal® in patients who did not respond to angioembolization. FloSeal® hemostatic matrix consists of a bovine-derived gelatin matrix component and a human-derived thrombin component, that replicate and augment the final stage of the coagulation cascade – the cleavage of fibrinogen into fibrin by the action of thrombin – when mixed together. The fibrinogen concentration of sealant is supraphysiologic, 15-25 times higher than that of circulating plasma. The resultant clot tends to form more rapidly and more reliably than normal. Other key components of fibrin sealant are Factor XIII, which covalently cross links the fibrin polymer to produce an insoluble fibrin coagulum, and an anti-fibrinolytic agent which inhibits fibrinolysis, thus preserving the stable fibrin clot.[20] Use of FloSeal® proved to be a graft-saving measure in both the patients which might have otherwise ended up in graft nephrectomy. Follow up over an average period of 10.4 months has shown stable renal parameters in each one of them. We have suggested the same treatment to other colleagues in different hospitals and the treatment was found to be successful.
Conclusion
Post-transplant renal biopsy bleeding is a common complication and most of the patients respond to conservative measures like bed rest, hydration, and blood transfusion or angioembolization. Lest the case does not respond to angioembolization, injection of a tissue sealant like FloSeal® hemostatic matrix in the biopsy tract should be tried. We conclude that such a procedure is safe and effectively controls the bleeding, thereby saving the patient from graft nephrectomy.
Source of Support: Nil
Conflict of Interest: None declared.
References
- The use of the automatic core biopsy system in percutaneous renal biopsies: A comparative study. Am J Kidney Dis. 1993;22:545-52.
- [Google Scholar]
- Management of non-neoplastic renal hemorrhage by transarterial embolization. Urology. 2009;74:522-6.
- [Google Scholar]
- Use of fibrin sealant as a hemostatic agent after liver biopsy in swine. J Vasc Interv Radiol. 2000;11:905-11.
- [Google Scholar]
- Incidence of bleeding after 15,181 percutaneous biopsies and the role of aspirin. Am J Roentgenol. 2010;194:784-9.
- [Google Scholar]
- Evaluation of complications due to percutaneous renal biopsy in allografts and native kidneys with color-coded Doppler sonography. Clin Nephrol. 1995;43:303-8.
- [Google Scholar]
- Complications of percutaneous renal biopsy: A review of 37 years› experience. Clin Nephrol. 1992;38:135-41.
- [Google Scholar]
- Safety of kidney biopsy in pediatric transplantation: A report of the controlled clinical trials in pediatric transplantation trial of induction therapy study group. Transplantation. 1999;67:544-7.
- [Google Scholar]
- Effects of superselective embolization for renal vascular injuries on renal parenchyma and function. Eur J Vasc Endovasc Surg. 2004;28:201-6.
- [Google Scholar]
- The role of interventional radiology in the management of blunt renal injury: A practical protocol. J Trauma. 2001;51:526-31.
- [Google Scholar]
- Percutaneous liver biopsy and track embolization with steel coils. Radiology. 1988;169:261-3.
- [Google Scholar]
- Fibrin sealant as a plug for the post liver biopsy needle track. Clin Radiol. 1989;40:627-8.
- [Google Scholar]
- Percutaneous transhepatic liver biopsy with tract embolization. Radiology. 1996;198:769-74.
- [Google Scholar]
- US-guided percutaneous liver biopsy with plugging of the needle track: A prospective study in 72 high-risk patients. Radiology. 1992;184:841-3.
- [Google Scholar]
- Hemostatic effect of glue-lipiodol mixture plugged in the needle tract after renal biopsies in a high-risk, anticoagulated rabbit model. Invest Radiol. 2000;35:684-8.
- [Google Scholar]
- Postbiopsy bleeding in a porcine model: Reduction with radio-frequency ablation–preliminary results. Radiology. 2003;227:493-9.
- [Google Scholar]
- Fibrin sealant enables tubeless percutaneous stone surgery. J Urol. 2004;172:166-9.
- [Google Scholar]
- Hemostatic agents and tissue glues in urologic injuries and wound healing. Urol Clin North Am. 2006;33:1-12.
- [Google Scholar]







