Translate this page into:
Partially thrombosed aneurysm of the abdominal aorta: Unusual cause of chronic inflammation and resistance to recombinant human erythropoietin
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Diagnosis of chronic inflammatory syndrome is often a challenge. In dialysis patients, this condition leads to resistance to recombinant human erythropoietin (rHuEPO). We here report a case of a 72-year-old male undergoing chronic hemodialysis and developed rHuEPO resistance without any obvious etiology. Investigations showed a partially thromosed aneurysm of the infrarenal aorta. Antiplatelet therapy was started with a satisfactory outcome.
Keywords
Aneurysm
atherosclerosis
chronic inflammatory syndrome
resistance to recombinant human erythropoietin
thrombosis
Introduction
Diagnosis of chronic inflammatory syndrome (CIS) is often a challenge in patients with chronic kidney disease. This condition also increases the risk of resistance to recombinant human erythropoietin (rHuEPO). We here report an uncommon etiology of CIS in hemodialysis and discuss its particularities.
Case Report
A 72-year-old male with nephroangiosclerosis was on maintenance hemodialysis (three sessions per week) for 10 years. He was a chronic smoker and had dyslipidemia treated with diet alone. His medications included: furosemide 500 mg in non-dialysis day, oral folic acid and vitamin B12, and monthly 75-150 μg of methoxy-polyethylene-glycol epoetin-beta. Biological monitoring revealed episodic elevations of C-reactive protein (CRP) ranging from 1 mg/l to 60 mg/l associated with a decrease of hemoglobin (Hb) levels without any other obvious cause of resistance to rHuEPO [Figure 1]. Serum ferritin, intact parathyroid hormone and aluminum levels were within the normal ranges. The mean Kt/v was 1.15. The patient had no malnutrition and his native fistula showed no malfunction.
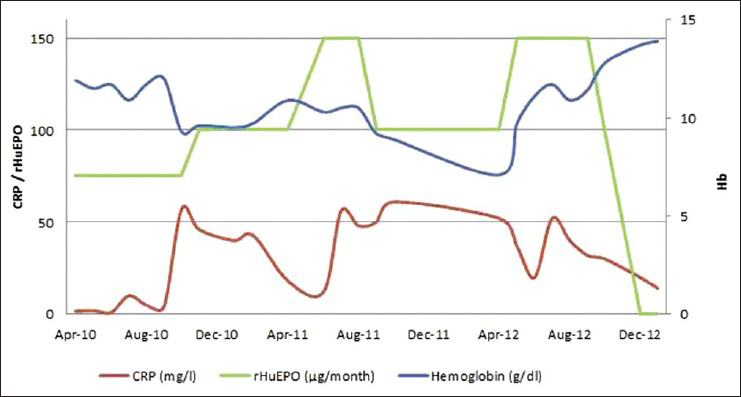
- History of inflammation, hemoglobin, and recombinant human erythropoietin doses
Physical examination found no evidence for any local or systemic cause of this inflammation. His vital signs were: Temperature 37°C, pulse 74 beats/min, blood pressure 128/68 mmHg and respiratory rate 20 breaths/min. Biological tests including liver parameters and serum protein electrophoresis were normal. Serology for hepatitis B virus showed negative hepatitis B surface (Hbs) antigen, positive anti-Hbs, and anti-hepatitis B core antibodies with no current biological or morphological signs of chronic hepatitis. Serology for syphilis, hepatitis C, and HIV viruses were negative. Chest radiography and radiography of the sinuses were normal. Sputum examination for acid-fast bacilli and tuberculin skin test was negative. The ear-nose-throat and stomatological examination were normal. Tumor markers were normal. Main laboratory tests are summarized in Table 1.

Transthoracic echocardiogram, blood culture, abdominal and pelvic ultrasound, eso-gastric endoscopy, and colonoscopy showed no abnormalities. As part of a screening study of vascular calcifications in hemodialysis, our patient underwent a lateral abdominal X-ray, which demonstrated diffuse calcifications of the abdominal aorta and a large aneurysm extending from the second to the fourth lumbar vertebra [Figure 2]. Multislice spiral computed tomography-angiography with 3D-reconstruction showed a saccular dilatation of the infrarenal segment of the abdominal aorta measuring 70 mm in height, 41 mm of anteroposterior diameter and 40 mm in transverse diameter with diffuse calcification of both anterior and posterior wall of the aorta extending to the primitive iliac arteries [Figure 3]. There was no evidence of dissection or rupture. Cross sections showed a partial thrombosis of the aorta wall [Figure 4]. The diagnosis of CIS complicating a partially thrombosed aneurysm of the abdominal aorta was then made. Antiplatelet therapy by lysine acetylsalicylate 160 mg/day was introduced to prevent embolic complications. Follow-up over last 6 months showed regression of inflammation, improvement of Hb level, and reduction of rHuEPO doses [Figure 1].

- Lateral abdominal X-ray: Aneurysm of the abdominal aorta

- 3D reconstruction of multislice computed tomography angiography: Extensive calcification of the abdominal aorta extending to the primitive iliac arteries

- Contrast enhanced multislice computed tomography angiography cross section: Partial thrombosis of the abdominal aorta wall
Discussion
Anemia is a common complication of chronic renal failure (CRF). Most patients with CRF achieve the desired target Hb level when supplemented with rHuEPO and parenteral iron.[1] About a quarter of the dialysis patients; however, have a poor response and need higher doses to reach the target Hb level.[2] Iron deficiency, underdialysis, infection and inflammatory conditions may all play a significant role in causing a poor response to rHuEPO therapy. Less common causes of resistance to rHuEPO include blood loss, hyperparathyroidism, aluminum toxicity, vitamin B12 or folic acid deficiency, hemolysis, marrow dysfunction, hemoglobinopathies, concomitant angiotensin converting enzyme inhibitor therapy, carnitine deficiency, and antibodies against the erythropoietin molecule.[34]
There is a well-demonstrated relationship between resistance to rHuEPO therapy and the inflammatory response.[567] Activation of the immune system during the inflammatory process diverts iron traffic from erythropoiesis to storage sites within the reticuloendothelial system, inhibits erythroid progenitor proliferation and differentiation, suppresses erythropoietin production, and blunts response to erythropoietin.[8] In clinical practice, measurement of CRP levels is widely used to monitor inflammation.[9] Our patient showed CIS without any evident etiology. Fortuitously, the diagnosis of partially thrombosed aneurysm of the abdominal aorta was made during a screening study and provided an explanation to this CIS.
Long duration on hemodialysis, advanced age, hypertension, dyslipidemia, and smoking are significant risk factors in our patient for atherosclerosis and vascular calcifications as reported in hemodialysis population.[10] The infrarenal abdominal aorta is prone to the development of atherosclerotic plaque and its complications including obstruction, ulceration, thrombus formation, and potentially, aneurysmal degeneration.[11] The spontaneous thrombosis of aortic aneurysm is rare.[12] In our patient, extensive atherosclerotic and calcified plaques may explain the thrombosis rather than the aneurysm itself.
Thrombosis and inflammation are intertwined in vascular pathology. Inflammation can beget local thrombosis, and thrombosis can amplify inflammation.[13] Indeed, the smooth muscle cell in the artery wall can undergo inflammatory activation when exposed to thrombin and products of thrombosis. For example, thrombin stimulation causes smooth muscle cells to produce interleukin (IL)-6 abundantly.[14] Platelet-derived growth factor, released from platelet alpha granules during thrombosis, can also markedly augment IL-6 production by smooth muscle cells.[15] IL-6, in turn, can induce the cute inflammatory phase response and increase plasma concentrations of fibrinogen, and the inflammatory marker CRP as in our patient. Thereby, antithrombotic treatment may suppress inflammation and help break the vicious cycle by limiting the local and systemic amplification loops between inflammation and thrombosis.[13]
Accelerated atherosclerosis and vascular calcifications are frequent, but ominous, complications in hemodialysis patients. The development of an aneurysm of the abdominal aorta is highly favored in this particularly exposed population. Functional signs are rare and often confused with digestive complaints. A CIS may accompany thrombotic complications and lead to resistance to rHuEPO. Our case alerts physicians on this rare etiology of CIS and highlights the importance of screening for vascular calcification in the early stages of kidney disease and during the hemodialysis follow-up.
Source of Support: Nil
Conflict of Interest: None declared.
References
- European best practice guidelines for the management of anemia in patients with chronic renal failure. Nephrol Dial Transplant. 1999;14(Suppl 5):1-50.
- [Google Scholar]
- Inflammation, serum C-reactive protein, and erythropoietin resistance. Nephrol Dial Transplant. 2001;16:224-7.
- [Google Scholar]
- Poor response to erythropoietin: Practical guidelines on investigation and management. Nephrol Dial Transplant. 1995;10:607-14.
- [Google Scholar]
- Hyporesponsiveness to recombinant human erythropoietin in dialysis patients. Dial Transplant. 2000;29:545-8.
- [Google Scholar]
- European best practice guidelines 14-16: Inadequate response to epoetin. Nephrol Dial Transplant. 2000;15(Suppl 4):43-50.
- [Google Scholar]
- High C-reactive protein is a strong predictor of resistance to erythropoietin in hemodialysis patients. Am J Kidney Dis. 1997;29:565-8.
- [Google Scholar]
- Effect of malnutrition-inflammation complex syndrome on EPO hyporesponsiveness in maintenance hemodialysis patients. Am J Kidney Dis. 2003;42:761-73.
- [Google Scholar]
- Cellular and molecular mechanisms of senescent erythrocyte phagocytosis by macrophages. A review. Biochimie. 1998;80:173-95.
- [Google Scholar]
- Inflammation and resistance to erythropoiesis-stimulating agents – What do we know and what needs to be clarified? Nephrol Dial Transplant. 2005;20(Suppl 8):82-7.
- [Google Scholar]
- Risk factors for atherosclerosis in patients with chronic kidney disease: Recognition and management. Curr Opin Pharmacol 2013 Epub ahead of print, in press
- [Google Scholar]
- Hemodynamic risk factors: Mechanical stress, mural architecture, medial nutrition and the vulnerability of arteries to atherosclerosis. In: Wissler RW, Geer JC, eds. The Pathogenesis of Atherosclerosis. Baltimore: Williams and Wilkins; 1972. p. :164.
- [Google Scholar]
- Thrombosed abdominal aortic aneurysms. Do they need surveillance to prevent late rupture? Eur J Vasc Endovasc Surg. 2001;22:570-2.
- [Google Scholar]
- Thrombin potently induces cytokine production by human vascular smooth muscle cells but not in mononuclear phagocytes. Circ Res. 1996;79:286-94.
- [Google Scholar]
- Proliferating or interleukin 1-activated human vascular smooth muscle cells secrete copious interleukin 6. J Clin Invest. 1990;85:731-8.
- [Google Scholar]







