Translate this page into:
Spontaneous Splenic Haematoma in a Patient on Hemodialysis: A Case Report
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Spontaneous splenic hematoma is one of the rare and life-threatening complications of chronic renal failure. The diagnosis of splenic hematoma is mostly made by imaging such as ultrasound or computed tomography. The management of spontaneous splenic hematoma is not standardized till now due to the rarity of this condition. Splenectomy is recommended in hemodynamically unstable patients with features of shock. This is a case report of spontaneous splenic hematoma in a patient with chronic renal failure. This case is reported due to the rarity with renal failure.
Keywords
Renal failure
shock
splenic hematoma
spontaneous
Introduction
Chronic kidney disease is associated with numerous complications, but spontaneous splenic hematoma is one of the rare and life-threatening complications of renal failure. Trauma is the most common cause for splenic hematoma, but in a subset of patients, hematoma occurs without history of trauma. The reported incidence ranges from 0.1% to 0.5%. Most of the cases are managed conservatively when a patient is hemodynamically stable. Splenectomy is only recommended for hemodynamically unstable patients.
Case Report
A 42-year-old male patient who was a known case of diabetes and chronic kidney disease was admitted with complaints of abdominal pain and vomiting for 4 days. There was no history of fever or trauma. The patient denied a history of tuberculosis, alcohol consumption, and anticoagulant use. He was on regular dialysis more than 6 months with heparin as anticoagulant for dialysis. 3000 units of heparin was used as loading dose followed by 1000 IU of heparin for maintenance dose. The last dialysis was done 2 weeks before the admission. On admission, the patient was drowsy and pale. His vitals were: Blood pressure 100/60 mmHg and pulse rate - 105/min. Abdominal examination showed tenderness in the left hypochondrium along with splenomegaly. Per rectal examination was normal.
On investigations, hemoglobin was 7.0 g/dl with raised renal parameters (urea 160 mg/dl and creatinine 12 mg/dl). Coagulation profile including prothrombin time, activated partial thromboplastin time, and international normalized ratio were normal. Ultrasound abdomen showed increased cortical echoes suggestive of chronic kidney disease with 6 cm × 8 cm perisplenic hematoma and hemoperitoneum. Computed tomography (CT) abdomen confirmed the 6 cm × 8 cm perisplenic hematoma with hemoperitoneum [Figures 1 and 2]. The patient was resuscitated with blood and blood product. During resuscitation, the patient did not show any sign of improvement, hence planned for emergency laparotomy. Intraoperative findings showed hemoperitoneum of 200 ml with ruptured spleen [Figures 3 and 4]. The ruptured spleen was adherent to adjacent structures. Spleen was completely removed and hemostasis secured. The patient developed left lower lobe atelectasis in the postoperative period, which improved with antibiotics and adequate physiotherapy [Figure 5].

- Computed tomography abdomen confirmed 6 cm × 8 cm perisplenic hematoma

- Computed tomography abdomen confirmed 6 cm × 8 cm perisplenic hematoma with hemoperitoneum

- Intraoperative findings showed hemoperitoneum of around 200 ml with adhesions

- Intraoperative findings showed completed ruptured spleen
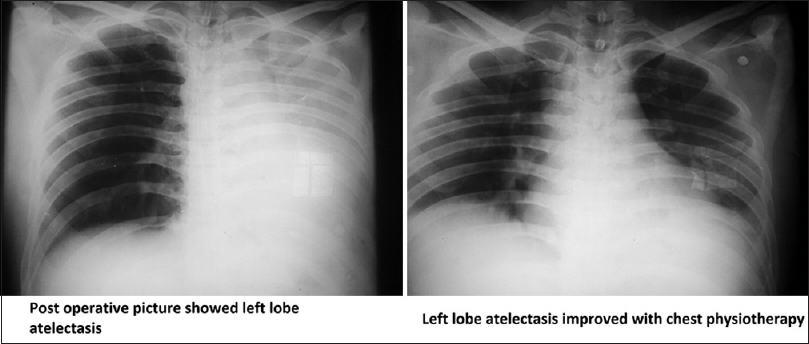
- Post operative chest X ray showed left lower lobe atelectasis which improved on chest physiotherapy
Discussion
Splenic hematoma is broadly classified as traumatic and nontraumatic splenic hematoma. Nontraumatic splenic hematoma is further classified as pathological splenic hematoma and spontaneous splenic hematoma.[1] It is considered pathological when postsplenectomy specimen showed abnormal pathological features whereas spontaneous when specimen showed normal histology.[2]
The proposed etiological factors for nontraumatic splenic hematoma include hematological malignancy (non-Hodgkin's lymphoma, acute and chronic leukemia), primary splenic malignancy, infectious condition (cytomegalovirus, Epstein–Bar virus, malaria, dengue, infectious mononucleosis, brucellosis, HIV, tuberculosis, babesia, bacillus, Q fever, influenza, aspergillus, typhoid), amyloidosis, drug-induced disorders (anticoagulant, antiplatelet, vemurafenib), and uremic coagulopathy.[3]
The mechanism of spontaneous splenic hematoma is not clear till now. There are proposed hypotheses such as increased intrasplenic pressure due to endothelial hyperplasia and vascular occlusion due to hypercoagulable state and spontaneous bleed from leaking capillaries.[4]
In most of the spontaneous splenic hematoma, there is splenomegaly. Splenomegaly is due to infiltration of malignant cells or congestion of the spleen. Incidence of splenic hematoma is higher in males as compared to females. Abdominal pain is the most common presenting complaint along with other nonspecific complaints. Blood investigations may show features of anemia along with underlying etiology. Systemic infections may be the cause for spontaneous splenic hematoma when routine investigations failed to identify the cause.[5]
The diagnosis of spontaneous splenic hematoma is mostly made by imaging by either ultrasound or CT.[6] Haemodynamic status plays a significant role in management strategy of spontaneous splenic haematoma. Those patients presented with features of shock or hemodynamic instability in spite of resuscitation are the candidates for splenectomy. Hemodynamically stable patient can be managed conservatively with blood transfusion and correction of underlying cause.[7] Serial ultrasound is mandatory for a patient on conservative management. Prognosis of spontaneous splenic hematoma depends on hemodynamic status and associated comorbid conditions.[8]
Conclusion
We suspect splenic hematoma when a renal failure patient presented with left hypochondrial pain. Ultrasound abdomen alone is sufficient for the diagnosis, but CT scan can be useful to exclude other intra-abdominal pathology. Hemodynamically stable patient can be managed conservatively. If a patient showed hemodynamic instability following resuscitation, splenectomy is warranted. A high index of suspicion is mandatory because early diagnosis saves patient's life.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Spontaneous splenic rupture in dengue fever with non-fatal outcome in an adult. J Infect Dev Ctries. 2012;6:369-72.
- [Google Scholar]
- Successful nonoperative management of spontaneous splenic hematoma and hemoperitoneum due to CMV infection. Case Rep Gastrointest Med. 2012;2012:328474.
- [Google Scholar]
- Spontaneous splenic rupture associated with apixaban: A case report. J Med Case Rep. 2016;10:217.
- [Google Scholar]
- Complicated malaria and a covert ruptured spleen: A case report. J Surg Case Rep. 2014;2014 pii: Rju122
- [Google Scholar]
- Hemoperitoneum from splenic rupture in an expatriate. J Emerg Trauma Shock. 2012;5:100-2.
- [Google Scholar]
- Characteristics of patients with spontaneous splenic rupture. Int Surg. 2014;99:714-8.
- [Google Scholar]
- Non-traumatic splenic rupture in a patient on oral anticoagulation. Int J Emerg Med. 2013;6:16.
- [Google Scholar]
- Spontaneous rupture of the spleen: A rare complication in a patient with lupus nephritis on hemodialysis. Saudi J Kidney Dis Transpl. 2010;21:712-4.
- [Google Scholar]







